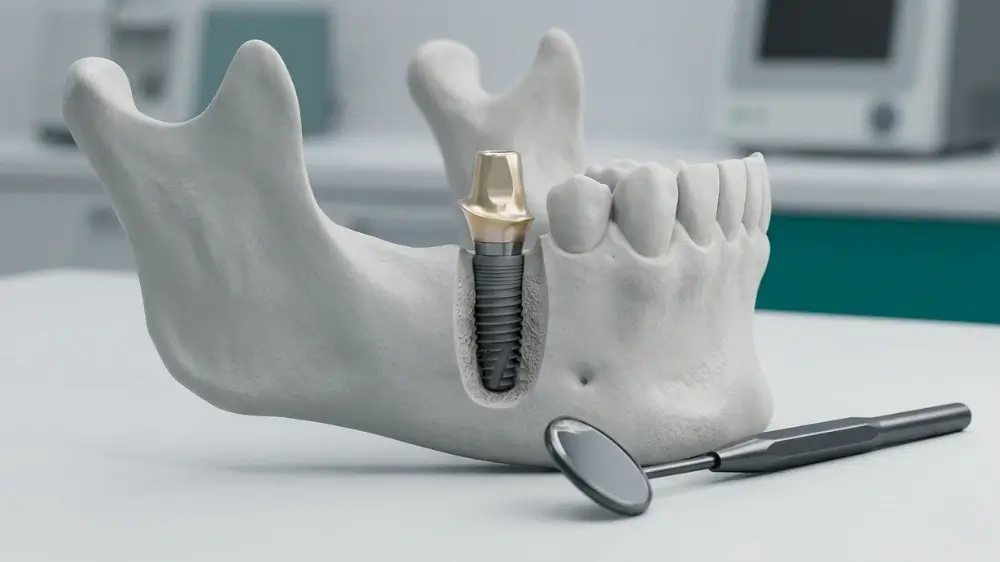
Dental implants are one of the most studied procedures in modern dentistry — and yes, dental implants are safe, provided you work with a qualified specialist and meet the clinical criteria. This being said, special patients require extra precaution: for example, diabetics and elderly +70 year old patients.
In this guide, Dr. Astolfi explores the most important factors to guarantee a smooth, seamless dental procedure; from how to know if your dental clinic ensures maximum safety, to how to guarantee the long-term success of your tooth implants.
What the science says at a glance:
- Dental implants have a 2% survival rate at 10 years, up from previous benchmarks thanks to advances in implant surface technology (Journal of Clinical Periodontology, 2024 DentalImplantOC)
- 4 out of 5 implants last 20+ yearswhen properly maintained — worldwide failure rate is just 3.1% Temeculaoralsurgery
- About 3 million dental implants are placed every year in the U.S. alone John Patterson, DMD, and the global market is projected to reach $9 billion by 2033
- Smokers are more than twice as likelyto experience implant failure compared to non-smokers (Sunflower Dental Spa, clinical data Sunflower Dental Spa) — the single biggest avoidable risk factor
Success Rate of Dental Implants
With a success rate of 98.6% at five years, 95% at 10-years and 80% after 20 years (when properly maintained), dental implants have one of the highest success rates of any surgical procedure in medicine. In fact, their reliability does nothing but increase over time.
For example: a 2024 meta-analysis puts the overall 10-year success rate at 95.2%, up from previous benchmarks — reflecting advances in implant surface technology and surgical technique. DentalImplantOC
Timeframe | Survival Rate |
5 years | ~98.6% |
10 years | ~95.2% |
20 years | ~88–92% (prospective studies) |
All-on-4 implants | ~98.8% cumulative |
Safety Protocols & Pre-OP Assessment: What a Reputable Clinic Must Do

The safety of dental implant surgery begins long before the operation. A thorough pre-operative assessment is the most important safeguard. It is also a great way of knowing whether your dental clinic meets all the latest safety criteria.
Here is what a rigorous pre-op protocol looks like:
- 3D CBCT scan (Cone Beam Computed Tomography): It provides clear 3D images that allow the surgeon to assess bone height, width, and density with precision. It also maps nerve pathways, preventing the nerve damage.
- Full medical history review: Blood thinners, bisphosphonates, immunosuppressants, and uncontrolled diabetes all directly affect healing and osseointegration.
- Blood tests: Particularly important for diabetic patients, where HbA1c levels must be assessed (ideally below 7–8%) before proceeding.
- Periodontal evaluation: Active gum disease is a contraindication for implants. Any existing infection must be treated and resolved first.
- Occlusion and bite analysis: Poorly planned implant positioning under excessive chewing force is a leading cause of late failure.
Dental Implant Surgery Step by Step
Dental implant surgery is a staged process typically spanning from 3 to 12 months — most of that time is simply your body healing, not clinical appointments.
Here is what the process looks like at each stage:
- Consultation & Imaging: Your surgeon reviews your medical history, takes a 3D CBCT scan, and assesses bone volume and density. If insufficient bone is present, a bone graft is planned first.
- Tooth Extraction (if needed): If the damaged tooth is still in place, it is removed. In some cases, the implant can be placed immediately at the same appointment (immediate implant placement), though this depends on bone quality and infection risk.
- Implant Placement: Under local anaesthesia, the surgeon makes a small incision in the gum and drills a precise channel into the jawbone. The titanium post is placed and the gum is sutured closed.
- Osseointegration: The implant fuses with your jawbone becomes part of your skeleton. Full osseointegration takes 3 to 6 months in the lower jaw, and up to 7 months in the upper jaw.
- Abutment Placement: Once osseointegration is confirmed, the surgeon reopens the gum to expose the implant head and attaches the abutment: a small connector that links the implant post to the final crown.
- Final Crown: Impressions are taken and sent to a dental laboratory, where your crown is custom-fabricated to match the colour, shape, and bite of your natural teeth.
Timeline at a glance:
Stage | Typical Duration |
Consultation & imaging | 1–2 appointments |
Bone graft (if needed) | +3–6 months healing |
Implant placement | 1 surgical appointment |
Osseointegration | 3–7 months |
Abutment & crown | 2–4 weeks |
Total (no graft needed) | ~4–8 months |
Total (with bone graft) | ~9–14 months |
How Painful Are Dental Implants?
Dental implant pain is considered mild. This is because the procedure is performed under local anaesthesia, so you feel no actual pain — only pressure and vibration.
After surgery: As anesthesia wears off, the true swelling and soreness kicks in. Most patients experience mild swelling, bruising, or soreness for 3 to 7 days, with the worst symptoms in the first 48 hours.
What the pain timeline looks like:
- Day 1–2: Peak discomfort. Swelling and soreness managed with ibuprofen or prescribed analgesics. Ice packs in 15-minute intervals recommended.
- Day 3–4: Swelling and pain begin to decrease noticeably.
- Day 5–7: Most patients are comfortable and back to normal routine.
- After 2 weeks: No pain expected. If pain or swelling persist beyond 14 days, contact your surgeon — this may indicate infection.
Main Benefits of Getting Tooth Implants
Dental implants have measurable, well-documented health benefits that no other tooth replacement option currently matches. We can summarize their main advantages in 5 key points:
- They prevent jawbone loss — permanently
When a tooth is lost, the jawbone beneath begins to disappear at a breathtaking pace. 30% of the alveolar ridge is lost in the first 6 months. Healthline Implants are the only solution that address this. A 10-year study found minimal bone loss around healthy implants — typically less than 0.2mm — which is clinically insignificant.
- They restore full chewing function
Implant-supported restorations improve bite force and chewing performance compared with removable prostheses, in many cases approaching the performance of natural dentition. Westhoustonperiodontics
- They protect adjacent teeth
A traditional dental bridge requires grinding down the two healthy teeth on either side of the gap to serve as anchors. Implants require no modification to neighbouring teeth whatsoever, preserving your remaining natural dentition.
- They are permanent and low-maintenance
Unlike dentures, implants are brushed and flossed exactly like natural teeth. Implants don’t get cavities and require only standard brushing and flossing. With proper maintenance, they can keep you smiling for at least 25 years.
- They preserve facial structure
Jawbone resorption after tooth loss causes the sunken, aged appearance seen in long-term denture wearers. By preserving bone volume, implants keep the face fuller and more youthful over the long term.
Dental Implant Risks
Dental implants are safe — but they are still surgery. According to a retrospective study assessing postoperative complications, the most common dental implant risks were infection, followed by peri-implantitis and implant failure. PubMed Central
Here are the risks that matter most:
Peri-implantitis: This is the most significant long-term risk. Peri-implantitis is a plaque-associated inflammatory condition affecting the tissue and bone surrounding a dental implant. Poor hygiene, smoking, and uncontrolled diabetes are the primary risk factors.
Infection: The most common short-term complication. Reputable clinics manage this risk with pre-operative antibiotic protocols and strict sterile surgical technique.
Nerve damage: Improper implant placement in the lower jaw can cause damage to the inferior alveolar nerve or trigeminal nerve. This risk is virtually eliminated by the use of 3D CBCT imaging.
Sinus complications: Relevant only for upper jaw implants. If the implant is placed too close to the sinus cavity without adequate bone height, it can protrude into the sinus and cause sinusitis.
Implant failure (osseointegration failure): Early implant failure occurs when the body does not successfully integrate the implant. Most early failures are biological: inadequate bone density, infection, or premature loading. The good news is that failed implants can almost always be replaced once the cause is addressed.
Potential Side Effects & How to Mitigate Them
Side effects after implant surgery are normal, expected, and — in the vast majority of cases — entirely manageable at home. The key is knowing what is a red flag requiring immediate clinical attention.
Common, expected side effects:
- Swelling: Swelling typically peaks around the second or third day before gradually diminishing — once it begins to go down, it should not increase again.
- Bruising: Mild discolouration on the face, cheeks, or neck is common and resolves within 7–10 days, just like any bruise.
- Bleeding: Light bleeding and blood-tinged saliva are common for the first day. Biting on gauze with gentle pressure for 20–30 minutes controls this effectively.
- Temporary numbness or tingling: Usually a result of local anaesthesia or minor nerve irritation. Notify your surgeon if numbness around the mouth or tongue persists beyond 5–7 days.
- Jaw stiffness: Common for several days post-surgery, especially with lower jaw implants. Ibuprofen helps manage both pain and stiffness simultaneously.
When to call your surgeon immediately:
- Pain that worsens after day 4 instead of improving
- Swelling that increases after day 3
- Fever above 38°C / 100.4°F
- Pus or discharge from the surgical site
- Persistent numbness beyond 7 days
- Any visible movement of the implant
Who Is Not a Proper Candidate for Dental Implants?
The best candidates have good overall health with sufficient jawbone density and healthy gum tissue without active periodontal disease. Here are the patients dentists will not consider suitable for the procedure:
- Patients with active, untreated gum disease
- Patients with uncontrolled diabetes (HbA1c above 8%)
- Patients currently undergoing head or neck radiation therapy
- Heavy smokers unwilling to stop around the surgical period
- Adolescents whose jaws are still growing
- Patients on high-dose intravenous bisphosphonates (osteoporosis medication)
Are Dental Implants Safe for The Elderly?
Yes — and the data is very reassuring. Patients over 75 actually showed higher five-year survival rates (96.8%) than the 65–75 age group (92.1%) according to an NIH study.
What does require special attention in older patients:
- Bone density: Age-related bone loss is common, and a bone graft may be needed before placement.
- Medications: Bisphosphonates (used to treat osteoporosis) carry a small risk of medication-related osteonecrosis of the jaw (MRONJ).
- Healing time: Osseointegration may take slightly longer in older patients..
- Systemic conditions: Cardiovascular conditions and diabetes are more prevalent in older patients — butmanageable with the right i care.
Are Dental Implant Safe for Diabetics?
Yes, provided your diabetes is well controlled. Diabetes affects wound healing and immune response, both of which are critical during osseointegration. A review found that diabetes, when well managed (HbA1c below 8%), does not compromise implant survival rates — with survival percentages ranging from 96.1% to 97.3% at one year and 87.3% to 96.1% at five years. nih
What this means in practice:
- HbA1c should ideally bebelow 7% before surgery; most surgeons will proceed up to 8%
- Blood glucose levels are monitored in the days around surgery
- Healing is monitored more closely, with more frequent follow-up appointments
- Antibiotic cover is standard protocol for diabetic patients
Are Dental Implants Safe for MRI?
Yes — modern titanium implants are fully MRI-compatible. Titanium implants are non-magnetic and do not pose a safety risk during scanning. They can sometimes cause small image distortions — called artifacts — near the implant site. But these are usually minor and do not compromise diagnostic quality.
What to do before an MRI:
- Inform your radiologist and MRI technician that you have dental implants
- Provide the implant brand and material if you have it (your surgeon can supply this)
- If your implants are older or of unknown material, ask your dentist to confirm compatibility first
How Safe Are Dental Implants in the Long Term?
Exceptionally safe — and the long-term data is among the strongest in all of reconstructive medicine. A study from the University of Gothenburg evaluated implants placed nearly 40 years ago — all implants remained in place and fully functional, demonstrating a 95.6% survival rate across nearly four decades. Loudfamilydentistry
It is worth understanding what degrades over time and what does not:
- The titanium post: Designed to last decades, often a lifetime.
- The abutment: Generally requires attention after 15–20 years.
- The crown: Subject to normal wear and tear, like natural teeth. Expect renewal after 10–15 years.
Are Dental Implants in Turkey Safe?
Yes, getting full mouth dental implants in Turkey is medically safe, provided the clinic adheres to international sterilization and surgical protocols. In 2026, Turkey has become a global leader in dental tourism, not just due to cost, but because of expertise and advanced digital dentistry. Safety for dental implants in Turkey is maximized through:
- The use of Grade 5 Medical Titanium and Zirconia from globally recognized brands.
- Implementation ofClass A sterilization environments to prevent cross-contamination.
- 3D Guided Surgery, which eliminates human error in implant placement.
FAQs
Can my body reject a dental implant?
Rejection does not happen because titanium is biocompatible and inert, meaning the immune system does not recognize it as a threat. “Failure” usually occurs due to poor bone quality, smoking, or infection (peri-implantitis).
How long does the safety of a dental implant last?
With proper maintenance, dental implants are designed to be a permanent solution. While the crown (the visible tooth) may need replacement after 10–15 years due to normal wear, the implant screw itself can remain safely integrated for 25 years to a lifetime.
What is the downside to dental implants?
The main downsides are cost, treatment time (3–12 months), and the surgical nature of the procedure. Rare complications include infection and peri-implantitis. However, no other tooth replacement option matches implants for longevity, function, or bone preservation.
Can a dental implant cause problems years later?
Yes — primarily peri-implantitis, a gum infection that causes progressive bone loss around the implant. Peri-implantitis incidence increases over time, reaching 7.1% at 8–10 years. It is largely preventable with good oral hygiene and regular professional check-ups.
Why would a dentist not recommend an implant?
Active gum disease, uncontrolled diabetes, insufficient bone volume, ongoing cancer treatment, or heavy smoking can make implants inadvisable — at least temporarily. Most of these are addressable before proceeding. A thorough clinical evaluation will clarify candidacy.
What is the failure rate of dental implants?
The worldwide average failure rate is 3.1%. Most failures occur early, during the osseointegration phase. Failed implants can usually be replaced successfully once the underlying cause — typically infection, bone insufficiency, or smoking — is identified and corrected.
What rots your teeth the fastest?
Frequent sugar consumption combined with poor oral hygiene is the fastest route to tooth decay. Sugary drinks — particularly sodas and fruit juices — are especially damaging as they bathe teeth in acid repeatedly throughout the day, accelerating enamel erosion and cavity formation.