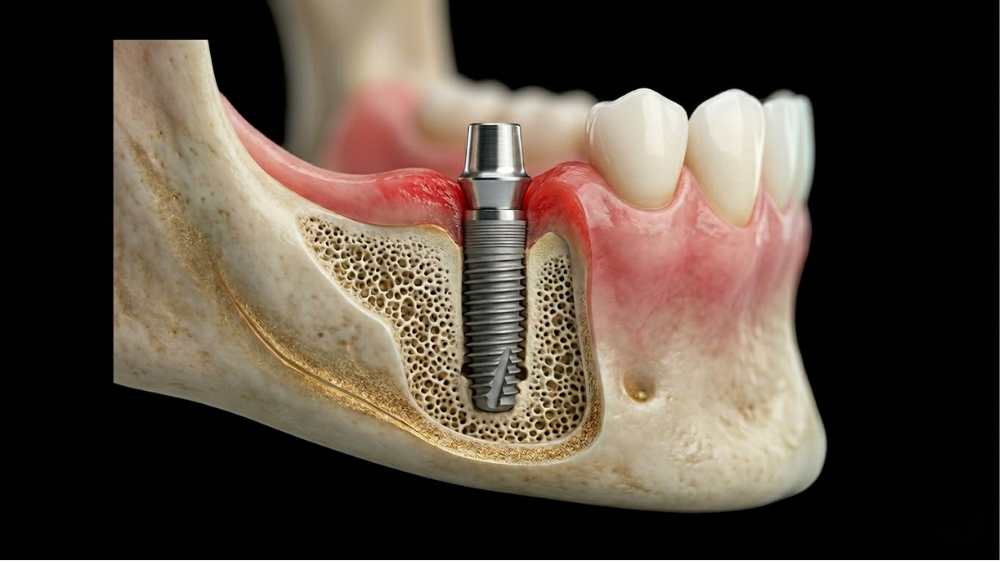
Losing a tooth to gum disease doesn’t have to be the end of your smile. Dental implants despite gum disease are an option. While infection is a hurdle, restoration is possible once we have the inflammation under control. By treating the underlying periodontitis, your new teeth can acquire the healthy foundation they need to last a lifetime.
How Gum Disease Affects Dental Implants
When we talk about gum disease, we are talking about the health of the “anchor” for your teeth. Periodontitis is an inflammatory infection that actively eats away at the jawbone and the connective tissues. Since a dental implant requires a sturdy bond with your bone to stay in place, any infection can become a major issue.
The primary risk is early implant failure. For a successful result, your bone must grow around the titanium implant and osseointegrate. If active bacteria are present during surgery, they can trigger an immune response that prevents this fusion. Furthermore, patients with a history of gum disease are more prone to peri-implantitis, a condition where the tissues around the implant become inflamed.
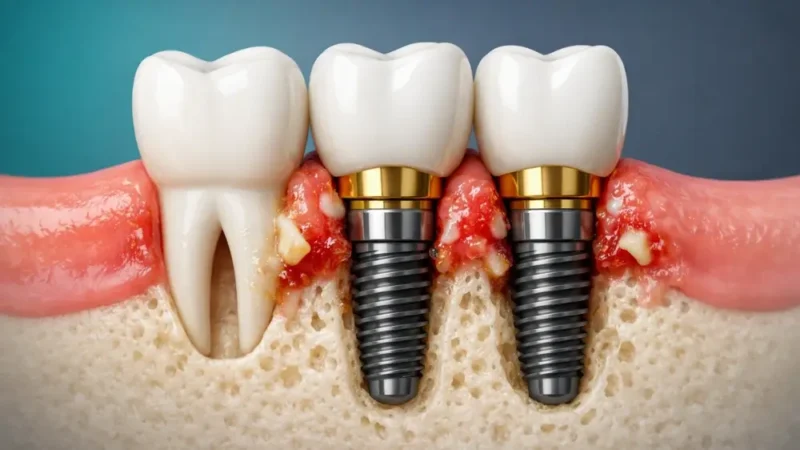
In Numbers: Dental Implants vs. Gum Disease
The success of dental implants is heavily supported by clinical data. While a history of periodontal disease adds a layer of complexity, the statistics show that with proper intervention, outcomes remain overwhelmingly positive. Modern dental protocols have evolved so that even those who have lost teeth to infection can achieve long-term stability.
Research indicates that for patients with a healthy oral history, implant success rates sit between 95% and 98%. For those with a history of treated and stabilized gum disease, the success rate remains high, typically around 90% to 92%. However, “treated” is the vital distinction; implants placed in an active infection zone face a drastically higher risk of failure.
Oral Health Condition | Success Rate (10-Year Mark) | Primary Risk Factor |
Healthy Gums | 98% | Mechanical Overload |
Treated Periodontitis | 92% | Peri-implantitis |
Active Gum Disease | < 70% | Failure of Osseointegration |
As the table illustrates, the difference between a successful restoration and failure often lies in pre-surgical preparation.
Preparing Your Gums for Restoration
The process involves a multi-step approach tailored to the severity of the bone and tissue loss. By following these steps, the inflammatory response is deactivated, allowing the body to focus its energy on osseointegration rather than fighting off bacteria.
Phase 1: Periodontal Therapy and Scaling
The first line of defense is scaling and root planing, often referred to as a “deep cleaning.” Unlike a standard cleaning, this procedure reaches far below the gum line to remove tartar and plaque from the pockets that have formed around the teeth. By smoothing the roots of the teeth, it becomes much harder for bacteria to re-attach.
In many cases, this is paired with antimicrobial therapy to eliminate any lingering pathogens. The goal of this phase is to achieve “pocket reduction.” When gums are healthy, they fit snugly around the tooth or implant. Forward progress only begins once those pockets have shrunk to a healthy depth of 3 millimeters or less.
Phase 2: Bone Grafting and Sinus Lifts
If gum disease has been present for a long time, it often leads to bone resorption. As an implant requires a specific volume of bone to stay secure, a thin or recessed jawbone must be reinforced. This is where bone grafting becomes essential. By placing specialized grafting material into the area of loss, the body is encouraged to regenerate its own bone structure.
For implants in the upper jaw, a sinus lift may be necessary if the sinus cavity is too close to the jawbone. This procedure gently adjusts the sinus membrane to create space for additional bone. While these steps extend the treatment timeline, they are the difference between an implant that fails within months and one that remains functional for decades.
Healthy Gums vs. Treated Periodontitis
Your maintenance plan is personalized to your oral health history. As shown in the below comparison, patients who have overcome periodontitis have a more proactive maintenance schedule. This ensures that any signs of recurring inflammation are identified before they can impact the implant’s stability.
Feature | Healthy Gums Baseline | Treated Periodontitis Baseline |
Gum Pocket Depth | 1–3 mm | 3 mm (Stable) |
Bone Density | Naturally sufficient | Often supplemented via Grafting |
Initial Healing Time | 3–4 months | 6–9 months (due to grafting) |
Maintenance Cycle | Every 6 months | Every 3–4 months |
Primary Goal | Integration | Infection Prevention & Integration |
Post-Implant Care: Preventing Peri-Implantitis
The biggest threat to an implant in a patient with a history of gum disease is peri-implantitis. This is an infection that attacks the tissues and bone surrounding the implant. Unlike a natural tooth, an implant does not have the same ligament barriers therefore infection can reach the bone more quickly.
The plan is simple; the hard part is just not skipping a day. Daily brushing and flossing are mandatory, but using specific tools like interdental brushes or water flossers can help reach the tight spaces around the implant crown. Regular check-ups allow for the monitoring of the soft tissue attachment, ensuring the seal around the titanium post remains tight and bacteria-free.
Who Cannot Have Dental Implants?
There are specific circumstances where dental implants may not be advisable. The primary goal is always a successful, long-term outcome, and certain health factors can significantly lower the chances of osseointegration.
- Uncontrolled Chronic Disease: Conditions like uncontrolled diabetes or autoimmune disorders can severely impair the body’s ability to heal after surgery and fight off potential infections.
- Active Periodontitis: As previously discussed, implants should never be placed in a mouth with active, untreated gum disease, as the bacterial load will likely lead to immediate failure.
- Heavy Smoking: Tobacco use constricts blood flow to the gums and bone, which is vital for healing. Statistics show that smokers have a significantly higher risk of implant rejection.
- Recent Radiation Therapy: Patients who have recently undergone radiation to the head or neck may have compromised bone density, making it difficult for the implant to bond.
- Severe Bone Loss without Grafting: If a patient has insufficient bone and is unwilling or unable to undergo bone grafting, there may not be enough physical structure to support the implant.
Frequently Asked Questions (FAQs)
Can I get dental implants if I currently have gum disease?
No, you cannot get implants while the infection is active. You must first undergo periodontal therapy to stabilize your gums. Once the infection is cleared and the inflammation is under control, the procedure can safely move forward.
How long does the process take if I need bone grafting first?
Adding a bone graft or a sinus lift usually adds about 3 to 6 months to the total treatment time. This allows the new bone to become strong enough to support the weight and pressure of an implant.
Is the procedure painful?
Most patients report that the procedure is less uncomfortable than a tooth extraction. Local anesthesia or sedation is used during the surgery, and any post-operative discomfort can typically be managed with standard over-the-counter pain relief.
Can implants get gum disease?
Yes. This is called peri-implantitis. It affects the gums and bone around the implant in the same way periodontitis affects natural teeth. This is why professional cleanings every 3 to 4 months are often recommended for patients with a history of gum disease.
What is the success rate for dental implants
For healthy patients, the success rate is around 98%. For those who have successfully treated their gum disease, the success rate remains very high, generally between 90% and 92%.