Dental implants are safe and successful in the overwhelming majority of cases. But they are still a surgical procedure — and like any surgery, they carry side effects, risks and potential complications.
This guide covers everything from the first few days post-op, to the serious complications that require immediate attention, and the long-term problems that can develop years later. We also explain what causes them, who is most at risk, and — most importantly — what you can do to prevent them.
If you have specific concerns about your own situation, Dr. Astolfi and OONE LIFE offer free dental consultations to patients requiring medical counsel.
Are Dental Implants Safe?
Yes — dental implants are one of the safest procedures in modern dentistry. Decades of clinical research confirm that, when placed by a qualified specialist, implants are a reliable, long-lasting solution for missing teeth. That said, they carry potential side effects and complications, like any surgical procedure.
What is the Success Rate of Dental Implants?
A study tracking over 10,800 implants across 4,247 patients found cumulative survival rates of 98.9% at 3 years, 98.5% at 5 years, and 96.8% at 10 years (French, Ofec & Levin, Clinical Implant Dentistry and Related Research, 2021). A 2024 meta-analysis published in Clinical Oral Investigations confirmed that roughly 4 out of 5 implants are still fully functional after 20 years (Kupka et al., Clinical Oral Investigations, 2024).
However, success rates depend on the patient’s health, lifestyle habits, bone quality, and — critically — the experience of the surgical team.
Dental Implants Side Effects & Complications
Before moving forward, let’s distinguish side effects of dental implants and complications (both can potentially happen post-op):
Side effects are temporary responses to dental implant surgery. Swelling, soreness and minor bleeding in the days after implant placement are normal.
Complications or problems are unintended problems that go beyond normal healing. They may be minor and easily treated — or, in rare cases, more serious. Some occur in the days immediately after surgery. Others can develop months or even years later.
Short-Term Side Effects of Dental Implants
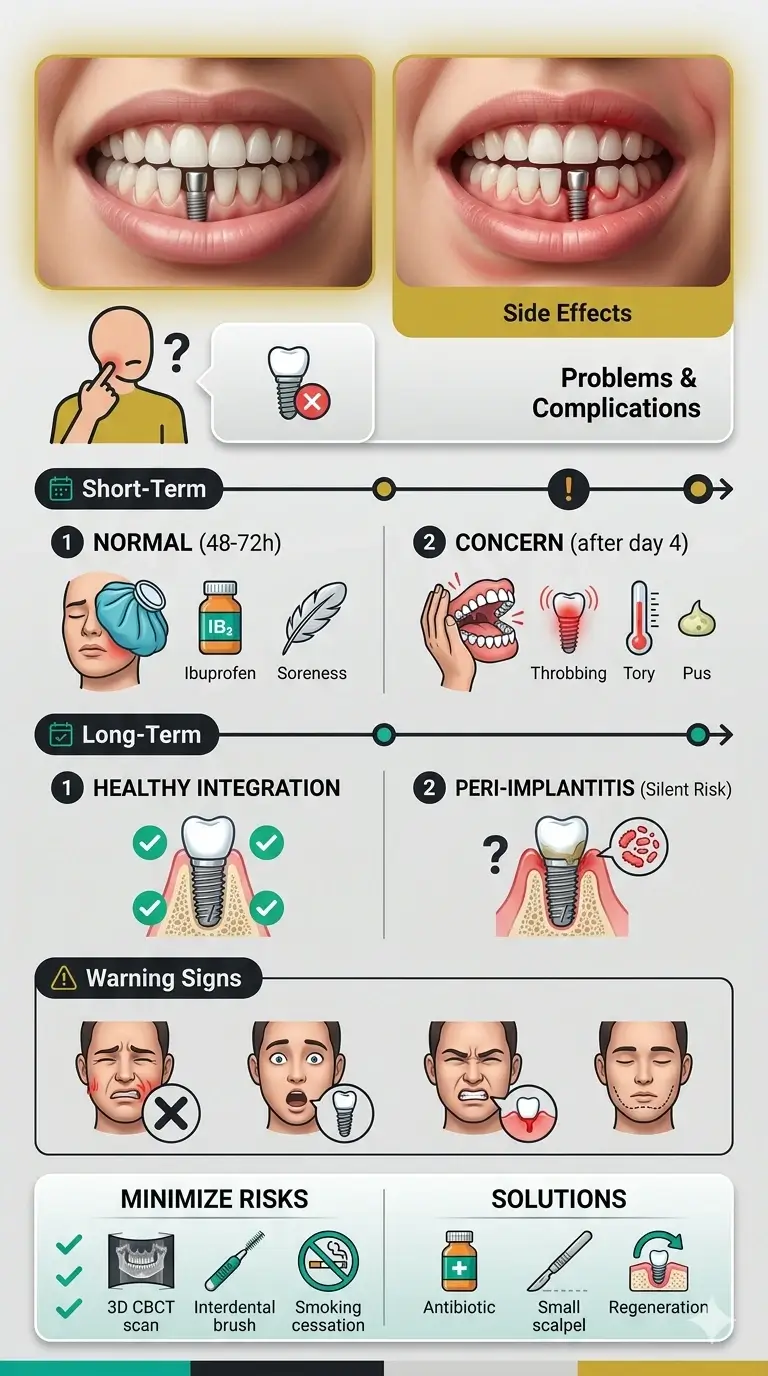
Getting a dental implant is oral surgery. That means some degree of discomfort is completely normal. It is not a sign that something has gone wrong. A study published in BMC Oral Health (2022) found that pain and swelling were each reported by 48.9% of patients on postoperative day 1 following dental implant surgery (Gu et al., BMC Oral Health, 2022), and in the vast majority of cases, these resolve on their own within 7–14 days.
Below, we will look at the most common side effects of dental implants, how to manage them and whether you should contact a dentist.
Pain & Soreness
Some soreness in the days following surgery is completely expected. For most patients, pain peaks within the first 48–72 hours and then improves steadily each day. It is usually managed with anti-inflammatories such as ibuprofen.
When to be concerned: Pain that intensifies after day four, or that does not respond to medication, is not a normal side effect. It may indicate an infection or a problem with osseointegration. Contact your dentist promptly — do not wait.
Swelling and Bruising
Swelling is your body’s natural response to surgery — it is a sign that healing is underway. It typically peaks at 48–72 hours, and gradually subsides over 7–10 days. Some patients also develop bruising on the face, jaw, or neck as blood disperses through soft tissue.
To manage swelling effectively:
- Apply an ice pack to the cheek for 20 minutes on, 20 minutes off during the first 24 hours
- After 48 hours, switch to warm compresses to promote circulation
- Keep your head elevated — even while sleeping — to reduce fluid accumulation
- Avoid strenuous physical activity for at least 7 days post-surgery
When to be concerned: Swelling that worsens after day three, spreads to other areas of the face, or is accompanied by fever, is not normal. These are potential signs of infection and require immediate attention.
Metallic Smell & Taste
Some patients notice a faint metallic taste or smell in the mouth in the first few days after surgery. This is generally caused by minor bleeding around the surgical site mixing with saliva, and it resolves as the wound closes and healing progresses.
When to be concerned: A temporary metallic taste is harmless. However, if it persists beyond the first week, worsens, or is accompanied by a bad taste, pus, or unusual odour, it may signal an early infection developing around the implant. This warrants a prompt check-up — caught early, infections are straightforward to treat.
Difficulty Chewing and Speaking
It is normal to feel some discomfort when chewing, and some patients notice a change in speech after the procedure. This happens because the surgical site is tender, and your mouth is adapting to a new structure. Stick to soft foods — yoghurt, mashed vegetables, eggs, fish — for the first week, and reintroduce firmer foods as comfort allows. Most patients return to a normal diet within a few weeks.
Speech adjustments typically resolve within days. If you have been fitted with a full-arch prosthesis such as All-on-4, an adaptation period is normal — your brain needs a little time to recalibrate.
At a Glance: What’s Normal vs. What Needs Attention
Symptom | Normal Duration | See a Dentist If… |
Pain & soreness | Peaks 48–72h, improves daily | Intensifies after day 4 or doesn’t respond to medication |
Swelling | Peaks 48–72h, gone by day 10 | Worsens after day 3 or spreads to face/neck |
Bruising | Fades over 7–14 days | Accompanied by hard lumps or spreading redness |
Difficulty chewing | 1–2 weeks | Persists beyond 3 weeks or is painful at rest |
Metallic taste | First 3–5 days | Persists beyond 7 days or accompanied by bad smell |
Rare But Serious Dental Implant Side Effects
The side effects covered in the previous section are common and temporary. The complications below are less frequent, but they require prompt attention when they occur.
Bleeding
Some light bleeding or blood-tinged saliva in the first 24 hours post-op is completely normal. It stops with gentle pressure and appropriate aftercare. Serious bleeding — where blood soaks through gauze pads or does not stop — is uncommon and should be checked immediately.
Patients on anticoagulant or antiplatelet medications face a far higher risk. In such cases, bleeding needs to be controlled so it does not lead to implant failure. If you are on blood thinners, always inform your surgeon before treatment.
Infection
Infection is the most serious complication of dental implant surgery. When infections occur and go untreated, the consequences are serious. A 2018 study found that 65% of infected implants ultimately had to be removed (Camps-Font et al., J Periodontol, 2018)
Signs of infection to watch for:
- Increasing pain after day 3–4 rather than improving
- Swelling that worsens or spreads
- Fever
- Pus or discharge from the surgical site
- Persistent bad taste or odour
Nerve or Tissue Damage
Nerve injury is genuinely rare when surgery is properly planned. The nerve most commonly at risk is the inferior alveolar nerve (IAN), running through the lower jaw. According to a review published in the Harvard School of Dental Medicine, nerve alterations take place in 12% of the cases in the first week, dropping to 5% after three months (Peña-Cardelles et al., Medicina Oral, 2025).
The critical factor: most nerve-related symptoms resolve within weeks to months. Permanent nerve damage is rare and strongly associated with inadequate pre-surgical imaging and inexperienced placement.
Symptoms that require immediate attention:
- Numbness or tingling that persists or worsens beyond a few weeks
- Sharp, shooting pain in the lip, chin or tongue
- Loss of sensation in any area of the lower face
If nerve involvement is suspected, contact your surgeon within 36 hours — early removal of the implant, if required, dramatically improves recovery outcomes.
Sinus Problems
Sinus complications are specific to upper jaw (maxillary) implants, where the roots of the back teeth sit close to the maxillary sinus cavities. If an implant is placed too deeply or without adequate bone height, it can perforate the sinus membrane or protrude into the sinus cavity.
The estimated failure rate of implants that perforated the sinus floor is 2.1%, and that the prevalence of sinusitis following such perforations was low (Corbella et al., MDPI, 2024). In other words, even when sinus membrane perforation occurs, it does not automatically lead to serious complications.
When sinus problems do develop, symptoms may include:
- Chronic pressure or congestion on one side of the face
- Recurring sinus infections
- A feeling of the implant “shifting”
- Nasal discharge on the affected side
Allergies
Dental implants are mostly made from titanium, a material chosen for its ability to integrate with human bone without triggering an immune response. True titanium allergy is exceptionally rare. Symptoms of a possible titanium reaction include:
- Chronic inflammation around the implant site that does not respond to standard treatment
- Persistent pain without clear clinical cause
- Skin reactions or generalised fatigue in rare cases
Testing options exist, including the MELISA® blood test for metal hypersensitivity. An alternative to titanium are zirconia tooth implants, a ceramic implant material that carries no metal allergy risk and is increasingly available at specialist clinics.
Problems & Complications of Dental Implants (Long-Term)
The dental implant complications below can develop months or even years after the procedure, often silently, with no obvious warning. This is precisely why regular check-ups and professional maintenance are what keep long-term oral health intact.
Failed Osseointegration
Osseointegration is the biological process by which the titanium implant fuses with the jawbone. When it fails, the implant must be removed.
Early osseointegration failure — before the implant is loaded with a crown or prosthesis — is the more common of the two types (seen in 2.73% of cases).
Late osseointegration failure — after loading (less than 0.3% of cases) — is less common but more complex. Typically caused by peri-implantitis, excessive bite force, or systemic health changes over time.
The main risk factors for osseointegration failure include:
- Smoking— consistently one of the strongest predictors across multiple studies
- Uncontrolled diabetes— impairs healing and bone metabolism
- Poor bone quality or density— particularly in the upper jaw
- Immediate loadingin cases where primary stability is insufficient
- Inexperienced surgical technique
Loose Implant
A dental implant that feels loose or mobile is a serious warning sign that should never be ignored. Looseness can originate in two places: the implant itself, or the crown or abutment.
A loose crown or abutment screw is easily fixed. A loose implant, however, indicates a failure of osseointegration or progressive bone loss around the implant — and it typically requires removal.
Causes of a loose implant include:
- Failed or lost osseointegration
- Advanced peri-implantitis eroding the surrounding bone
- Biomechanical overload — for example in patients with bruxism (teeth grinding)
- Trauma or impact to the jaw
What is the Most Common Long-Term Complication of Dental Implants? Peri-Implantitis
Peri-implantitis is the single most common long-term complication of dental implants — and the leading cause of late implant failure. It is a bacterial infection of the tissue and bone surrounding the implant.
Approximately 1 in 5 implant patients develops peri-implantitis, with an incidence rate of 22% over 20 years — Galarraga-Vinueza et al., J Periodontol, 2025. Peri-implantitis progresses in a non-linear, accelerating pattern: it can remain manageable for years, then deteriorate rapidly.
Signs of peri-implantitis:
- Bleeding or swelling of the gum around the implant
- Bad breath or persistent bad taste
- Deepening pocket around the implant on probing
- Visible bone loss on X-ray
- In advanced cases, implant looseness
Gum Recession and Bone Loss
Over time, the gum tissue and bone around a dental implant can recede — exposing part of the implant. It is one of the most aesthetically troubling long-term complications, particularly for front teeth.
Peri-implant soft tissue dehiscence occurs in 33.3% of cases within the first year, rising to 38.3% at 3–5 years and 64.5% beyond 5 years — Wang et al., J Periodontol, 2025. These figures include minor as well as significant recession, and do not all represent clinical failures — but they underline that soft tissue stability around implants requires active monitoring.
Problems with All-on-4 Dental Implants
The clinical data is reassuring on overall survival. Industry statistics and multiple clinical studies report a survival rate of approximately 98.8% for All-on-4 over 5–10 years — comparable to or better than many individual implant studies. However, specific complications do occur and are worth understanding:
- Screw loosening or fracture— one of the more common mechanical issues, particularly in the first year, usually resolved with a straightforward clinical adjustment
- Prosthesis fracture— the full-arch bridge is under significant occlusal load; fractures can occur, especially in patients with bruxism
- Peri-implantitis— affects All-on-4 patients as it does single-implant patients, but the consequences are higher-stakes given that four implants support the entire arch
- Bone resorption under the prosthesis— loss of residual ridge bone beneath the prosthetic teeth can occur over time, affecting fit and aesthetics
Complications with 3-on-6 Dental Implants
The 3-on-6 system remains a clinically sound option. Its complications are manageable with diligent aftercare. As with All-on-4, the experience of the surgical team is decisive in long-term success.
Specific complications to be aware of with 3-on-6 include:
- More complex surgery
- Fracture or debonding
- Uneven load distribution
- Higher maintenance
Warning Signs NOT to Ignore — When to See a Dentist
A well-integrated implant should feel like a natural tooth. If something feels off, that instinct is worth acting on. The details beneath explains what each symptom may indicate and how urgently you should act.
Warning Sign | Possible Cause | Action |
Pain that worsens after day 4 | Infection, failed osseointegration | Contact dentist within 24 hours |
Swelling that spreads or returns | Infection, abscess | Contact dentist within 24 hours |
Implant feels loose or mobile | Failed osseointegration, bone loss | Contact dentist immediately |
Bleeding gums around the implant | Peri-implant mucositis, peri-implantitis | Book appointment within days |
Persistent bad taste or odour | Bacterial infection, peri-implantitis | Book appointment within days |
Visible metal or gap at gumline | Gum recession, peri-implantitis | Book appointment within days |
Numbness or tingling that persists | Nerve involvement | Contact dentist within 24–48 hours |
Fever alongside any implant symptom | Systemic infection | Contact dentist same day |
Bite feels different or uneven | Mechanical issue, implant shift | Book appointment within days |
Factors Leading to Dental Implant Complications
Some of these factors are within your control. Others require careful clinical planning before surgery ever begins. Risk factor for dental implant complications:
- Smoking
- Uncontrolled diabetes
- Bruxism
- Poor oral hygiene
- History of periodontitis
- Poor bone health
- Radiotherapy
- Certain medications
- Age over 60
- Inexperienced surgeon/clinic
Prevention & Aftercare: How to Minimize Risks
The evidence on dental implant complications points consistently in one direction: most failures are preventable. The combination of thorough pre-surgical planning, appropriate patient selection, and consistent long-term maintenance eliminates the vast majority of risk factors discussed in this article.
Before Surgery
A clinic that rushes to treatment without comprehensive assessment is a clinic that cuts corners on the most important part: a proper pre-surgical workup. This should include:
- Full medical history review— including all medications, systemic conditions, history of periodontitis, and lifestyle factors such as smoking
- 3D CBCT imaging— cone beam computed tomography gives the surgeon a precise three-dimensional map of your bone density, bone volume, nerve location and sinus position. It is the single most important tool for preventing nerve injury and sinus perforation.
- Treatment of any active gum disease— placing an implant into a mouth with uncontrolled periodontitis significantly increases the risk of peri-implantitis.
- Smoking cessation— ideally several weeks before surgery and continuing for at least 8 weeks post-surgery.
- Optimising systemic health— diabetic patients should target optimal HbA1c levels; patients on bisphosphonates or other high-risk medications should discuss with their surgeon
After Surgery: The First Two Weeks
The early healing phase is critical. Osseointegration begins immediately and is most vulnerable in the first few weeks. Aftercare in the immediate post-op must include:
- Chlorhexidine mouthwash (0.12%)for the first two weeks
- Soft diet— avoid hard, crunchy or chewy foods
- No smoking— absolutely critical during the osseointegration phase
- No exercisefor at least one week
- No straws or brushing— suction and pressure can disturb the clot at the surgical site
- Take prescribed antibiotics and pain medication as directed— do not stop the course early
Long-Term Maintenance
Preventive measures must begin before implant placement and continue throughout a patient’s lifetime. Daily home care routines that should be zealously followed include:
- Brush twice daily
- Clean interdentally every day
- Avoid tobacco
Professional Maintenance
Maintenance visits for implant patients should be scheduled every 6 months. At every maintenance visit, your clinician should assess:
- Gum health around each implant
- Presence of bleeding or suppuration
- Implant stability and occlusion
- Radiographic bone levels
If you have bruxism: wear your nightguard every night without exception.
Solutions for Dental Implant Problems
The vast majority of dental implant problems can be treated effectively when caught early. Even in cases where an implant must be removed, the story rarely ends there.
Solutions for Side Effects of Dental Implants
The temporary side effects of pain, swelling, bruising, immediately post-op, require no intervention beyond what your surgeon prescribes. Standard management includes:
- Prescribedpainkillers (ibuprofen) for pain and inflammation
- Ice packs
- Chlorhexidine mouthwasht
- Soft diet and restduring the first 7–10 days
Early infection: antibiotics and professional cleaning
Infections caught in the first weeks after surgery are the most straightforward to treat. The typical approach involves:
- Antibiotic therapy
- Professional debridementof the implant site to remove bacterial biofilm
- Antiseptic rinseswith 0.12–0.2% chlorhexidine
How to Cure Peri-implantitis
Peri-implantitis treatment escalates from non-surgical to surgical depending on severity.
Stage 1 — Non-surgical therapy (mild to moderate disease):
- Removal of plaque, calculus and biofilm from the implant surface
- Chlorhexidine gel or antibiotics
- Improved patient oral hygiene
Stage 2 — Surgical therapy
When bone loss is significant, surgery is required. The primary goal is to access and decontaminate the implant surface and eliminate deep peri-implant pockets. The main surgical options are:
- Access flap debridement— A five-year study cited in the British Dental Journal found 54% of implants treated with resective surgery achieved successful disease resolution — Roccuzzo et al., Br Dent J, 2024
- Regenerative surgery with bone grafting— bone graft material and barrier membranes can be used to regenerate lost bone and attempt re-osseointegration
- Implantoplasty— smoothing and polishing of the exposed implant threads to reduce bacterial adhesion surface and facilitate tissue healing
Nerve-related dental implant complications
Permanent nerve damage is rare and associated with inadequate pre-surgical imaging. At specialist clinics using CBCT-scans, this complication is largely preventable. In case symptoms appear — numbness, tingling or altered sensation — the treatment approach depends on severity and timing:
- Immediate repositioning or removal
- Anti-inflammatory medication
- Vitamin B complex supplementation
- Monitoring and neurosensory testing
Implant removal and replacement
Removal is a straightforward procedure performed under local anaesthesia. After removal, the site is cleaned and allowed to heal. In many cases a new implant can be placed after healing — typically 3–6 months post-op. In case of bone loss, a bone graft is performed.
- Replacement implants have a success rate of approximately 90%
How Many Times Can a Dental Implant Be Replaced?
There is no fixed upper limit. Technically, a site can be reimplanted multiple times provided sufficient bone volume and patient health. In practice, however, each successive failure makes the next attempt progressively more challenging.
- First replacement: strong odds of success 88.7%— compared to 98.6% for initial implants — Siow et al., PMC, 2022.
- Second and third replacements: cumulative survival of 67.1% —Siow et al., PMC, 2022
What Can Be Done Instead of a Dental Implant?
Not every patient is a suitable candidate for dental implants. Some people have insufficient bone, uncontrolled medical conditions, or personal or financial reasons to consider alternatives. The three best are dental bridges, removable partial dentures, and full dentures. None of them, however, matches the long-term performance and benefits of implants.
Dental bridges
It is a non-surgical option that can be placed relatively quickly and at lower upfront cost than an implant. The trade-offs are significant, however. The healthy adjacent teeth must be filed down to accept crowns. Over time, abutment teeth are placed under additional load, increasing their vulnerability to decay, fracture and root canal problems.
Removable partial dentures
It is the least invasive and least expensive option — but also the least functional and least durable. RPDs do not prevent bone loss at the missing tooth site. They require regular relining as bone changes shape, and patients often report reduced chewing efficiency, discomfort, and the social and psychological inconvenience of a removable appliance.
Full dentures
For patients who have lost all or most of their teeth, conventional full dentures remain an accessible option. They require no surgery and carry no medical risk of the kind associated with implant placement. However, they come with well-documented limitations: instability during chewing and speaking, ongoing bone resorption leading to progressive changes in facial structure, and the need for adhesives and regular adjustments.
Implant-supported dentures — also known as implant overdentures — represent a meaningful upgrade.
Comparison: Implants vs. Alternatives
Implant | Bridge | Partial denture | Full denture | |
10-year survival | ~97% | ~89% | Lower | Varies |
Prevents bone loss | ✅ Yes | ❌ No | ❌ No | ❌ No |
Affects adjacent teeth | ❌ No | ✅ Yes | ✅ Partially | ❌ No |
Feels like natural tooth | ✅ Yes | Partial | ❌ No | ❌ No |
Removable | ❌ No | ❌ No | ✅ Yes | ✅ Yes |
Lifespan | Potentially lifetime | 10–15 years | 3–7 years | Requires adjustment |
Upfront cost | Higher | Moderate | Lower | Lower |
Long-term cost | Lower | Higher (replacement) | Higher (maintenance) | Higher (adjustment) |
Do Dental Implants in Turkey Have More Side Effects?
Turkey is one of the world’s most established destinations for medical tourism. The country’s dental sector includes clinics operating to ISO and international accreditation standards, using the same premium implant brands — Straumann, Nobel Biocare, Astra Tech — used in top clinics across Europe and the US. Many Turkish oral surgeons have trained internationally and hold postgraduate specialist qualifications.
For patients considering dental implants in Turkey, the key is to distinguish between high-volume budget clinics and specialist implant centres operating to international standards.
FAQs
How long do dental implants last?
The titanium post can last a lifetime with proper care. The crown attached to it typically needs replacing after 10–15 years due to normal wear. Long-term survival depends heavily on oral hygiene and regular professional maintenance.
What are the symptoms of a failing dental implant?
Key warning signs include: pain that worsens after day four, a loose or mobile implant, swelling that returns, bleeding gums, persistent bad taste or odour, visible metal at the gumline, and numbness that doesn’t resolve.
What is the biggest problem with dental implants?
Peri-implantitis — a bacterial infection of the tissue and bone surrounding the implant — is the most common long-term problem. It affects approximately 1 in 5 patients over 20 years, but is largely preventable with consistent maintenance.
How do you know if your implant is rejecting?
True titanium rejection is extremely rare. What patients call “rejection” is usually failed osseointegration or peri-implantitis. Signs include persistent pain, mobility and swelling. A clinical assessment — not waiting — is the right response.
What are the dangers of getting a tooth implant?
The main dangers are post-operative infection, peri-implantitis developing over time, nerve injury if placed without adequate imaging, and sinus complications for upper jaw implants. All are substantially reduced by specialist surgical care and thorough pre-surgical planning.
Can a dental implant cause problems years later?
Yes. Peri-implantitis, gum recession and bone loss can develop silently long after a successful procedure. This is precisely why professional maintenance every 3–6 months is not optional — it is how late complications are caught before they become irreversible.
Why does my tooth implant hurt years later?
Late implant pain usually signals developing peri-implantitis, a loose abutment screw, bite changes causing mechanical overload, or rarely a nerve issue. Do not assume it will resolve on its own — it rarely does, and delay makes treatment harder.
Does anyone regret getting dental implants?
Most patients do not. Satisfaction rates are consistently high across clinical studies. Regret is most common when complications go unaddressed or expectations weren’t set clearly. Honest pre-treatment counselling and a reliable aftercare plan are as important as the surgery itself.