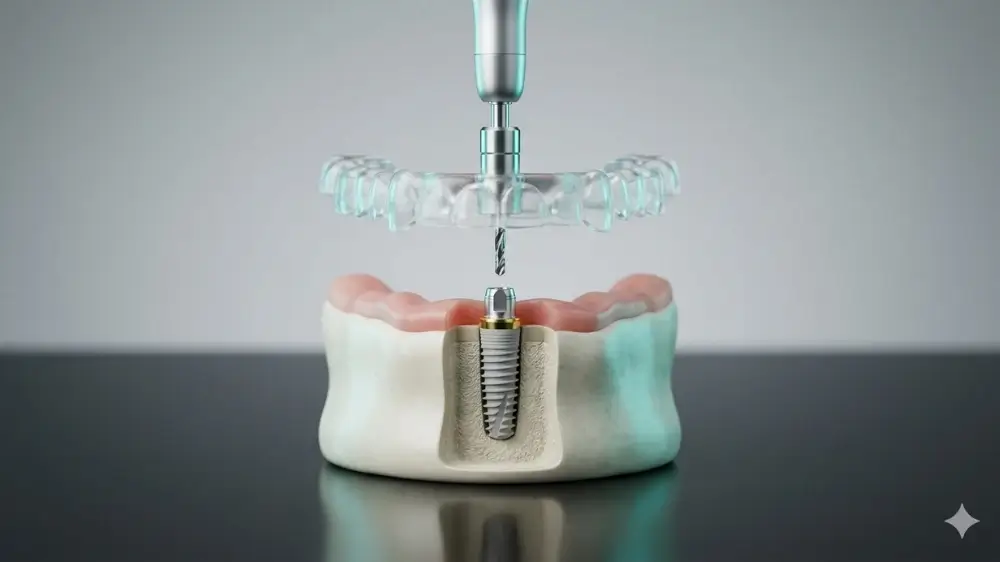
A dental implant reconstructs the entire tooth structure: the visible enamel and the root beneath the gum. In this guide, we walk you through every stage of the tooth implant process, from the first diagnostic scan to the placement of your final crown. Each section is grounded in years of clinical experience, so you know exactly how painful the process is, and what to expect from dental implants surgery.
Key facts at a glance:
- The 10-year survival rate for dental implants is 4% (95% CI: 95.2%–97.5%), according to a systematic review and meta-analysis of 18 clinical studies. PubMed
- 4 out of 5 implantswill last 20 years or more when properly maintained. Temeculaoralsurgery
- The global dental implant market is valued at approximately$8 billion (2026), reflecting high demand worldwide. Impressions Dental
What Is the Pain Scale for Dental Implants?
Most patients rate implant surgery at 2–3 out of 10 on a pain scale. Fear of pain is the primary reason why patients delay treatment. Yet, the tooth implants process itself is painless. Surgery is performed under local anaesthesia. You will feel pressure and movement, but no pain. For anxious patients, needleless anesthesia is available, too. Overall, patients often say that dental implants are much less uncomfortable than a tooth extraction.
How Long Does the Dental Implant Surgery Take?
Dental implants surgery takes anywhere from 20 minutes to 4+ hours. It depends on the number of implants and the complexity of the case. As a reference, a single implant can be placed in 20-45 minutes, whereas all-on-4 dental implants can take 2.5-4 hours per arch.
Are You a Candidate for Dental Implants?
Most healthy adults who are missing one or more teeth are candidates. The decisive factor is your bone volume and health. A clinical assessment is required before any treatment plan is confirmed.
Good candidates typically present with:
- Sufficient jawbone density and height to anchor the implant fixture
- Healthy gum tissue with no active periodontal disease
- No uncontrolled systemic conditions (e.g., unmanaged diabetes)
- Non-smoker status, or willingness to quit during the healing phase
Tooth Implants Process Step by Step
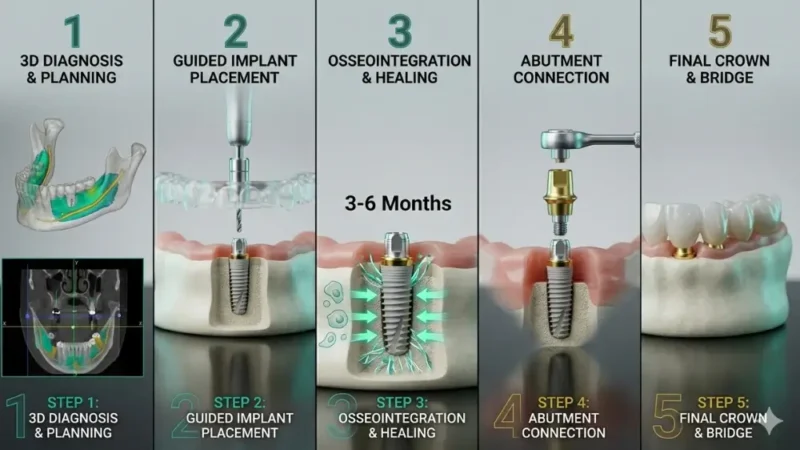
Dental implants surgery can last up to +4.5 hours in case of full mouth dental implants, or as little as 1h for single implant placement. The procedure is performed entirely under anesthesia, with medication provided before sedation subsides.
1. Diagnosis and Treatment Planning
Every major surgical decision (implant size, angle, depth, proximity to nerves), is made here. At OONE LIFE DENTAL, we advise patients to choose clinics using a fully digital workflow, eliminating the guesswork and anatomical risk from traditional 2D X-ray planning.
CBCT Scan for 3D Mouth Mapping
A Cone Beam Computed Tomography (CBCT) scan produces a precise, 3D map including your bone density, the location of your nerves, and the boundaries of your sinus cavities. Approximately 36% of implant surgeries now incorporate 3D CBCT imaging, a number increasing year by year for obvious reasons.
What the digital planning delivers:
- A virtual surgery performed in software before the real one
- Implant size and angulation selected to the nearest 0.1°
- A 3D-printed surgical guide used on the day of surgery to transfer the digital plan directly into the patient’s mouth
- Identification and avoidance of all critical anatomical structures
The result is a procedure that is faster, safer and with a smoother recovery.
2. Bone Grafting
When the CBCT scan reveals insufficient jawbone for dental implants, bone grafting is needed. This is unavoidable, as the implant fixture requires a minimum volume of stable bone to achieve osseointegration.
The two most common preparatory procedures are:
- Bone Grafting: Adds bone material (synthetic, animal-derived, or autologous) to the required areas of the jaw.
- Sinus Lift: Specific to the upper jaw. The sinus membrane is surgically elevated and bone material is added beneath it.
3. Implant Placement
The surgical phase of the tooth implants process. It involves sedation, drilling and prosthetic placement on top of the fixture. It usually lasts 20 minutes to +4 hours.
- Anaesthesia: Local anaesthesia is administered to fully numb the treatment area. You remain awake and comfortable throughout. For patients with dental anxiety, conscious sedation is available as an adjunct.
- Surgical Mold (Dental Guide): The custom surgical guide (produced from your CBCT scan data), is seated over your gum tissue. This template contains pre-drilled channels that physically constrain the drill to the exact angle, position, and depth determined during digital planning.
- Placing the Titanium Fixture: A small incision is made in the gum tissue to expose the bone. The surgeon drills a channel and seats the titanium implantinto the jawbone. In some guided surgery cases, sutures are not required, or only 2–3 absorbable stitches are placed.
- Temporary Crown: Once the fixture is in place, either a healing cap or a temporary crownis attached. For full-arch cases, a fixed temporary bridge is typically delivered the same day.
4. Osseointegration & Healing
Osseointegration takes 3 to 6 months. This is the usual waiting time between the moment implants are placed and when your final crowns are fitted. This timeline cannot be shortened and attempting to do so is the most common cause of implant failure.
How Long Does Healing Take After a Dental Implant?
Full healing after a dental implant takes 3 to 6 months. Initial gum soreness and swelling subside within 7 to 10 days, while osseointegration requires several months before the final crowns can be attached.
- Phase 1: Soft Tissue Recovery (Days 1–14):During the first 48–72 hours, patients experience peak swelling and minor discomfort. By the end of the second week, the surgical site is usually closed, and stitches are removed.
- Phase 2: Osseointegration (Months 3–6):This is the mandatory waiting period.
Osseointegration Timeline
The osseointegration timeline unfolds in biological phases, each with specific tissue-level activity:
What Is Clinically Happening | ||
Initial healing | Hours 1–72 | Blood clot forms at the bone-implant interface; bone begins repair response |
Soft tissue healing | Weeks 2–6 | Gum tissue around the implant site begins closing and consolidating |
Early osseointegration | Weeks 6–12 | New bone formation is observed on the implant surface; by 8–12 weeks, the peri-implant interface begins to be replaced by mature lamellar bone in direct contact with the implant surface |
Maturation | Months 3–6 | Immature bone tissue undergoes full bone remodelling, replaced by durable, load-bearing mature bone tissue |
Full integration confirmed | Month 5–6+ | Stability confirmed via X-ray; permanent crown or bridge can be placed |
5. Abutment and Final Crowns
This is the appointment patients look forward to most. Once osseointegration is confirmed, the permanent restoration is attached. The implant process is, at this point, complete.
The appointment proceeds as follows:
- Osseointegration Confirmation: Your surgeon verifies full bone-implant fusion through radiographic imaging and a physical stability test. No crown is placed until this is confirmed without exception.
- Abutment Connection: The temporary healing cap is removed. The abutment, a connector piece in titanium, zirconia, or gold alloy, is screwed directly into the implant fixture and torqued to the manufacturer’s specified value. This is a brief, entirely painless procedure.
- Final Crown or Bridge: The permanent crown or bridge is custom-milled to match your bite, tooth colour, and anatomy. At this final stage, it is secured to the abutment.
Dental Implant Success Rate
Dental implants are the most validated tooth replacement in modern dentistry. The evidence spans decades of peer-reviewed research across tens of thousands of patients. We have yet to find a better solution.
The key figures, sourced from clinical literature:
- A large study of 10,871 implants in 4,247 patients followed for up to 22 years reported survival rates of 9% at 3 years, 98.5% at 5 years, and 96.8% at 10 years.
- The cumulative prosthetic survival rate for All-on-4 full-arch restorations specifically is 8%. Impressions Dental
- Over a 20-year horizon, a 2024 meta-analysis published inClinical Oral Investigations confirms that 4 out of 5 implants placed with modern rough-surface titanium fixtures can be expected to survive.
What Can Cause a Dental Implant to Fail?
Implant failure is uncommon, but it is not random. The vast majority of failures are attributable to preventable factors and fall into two categories:
Early failure
Occurs during the osseointegration phase (months 1–6) and is typically caused by:
- Poor surgery / incorrect positioning
- Insufficient bone volume not identified pre-op
- Placing a crown before osseointegration is complete (premature loading)
- Active infection at the surgical site
- Smoking during the healing phase
Late failure
Occurs after successful osseointegration and is almost exclusively caused by:
- Peri-implantitis — a progressive bacterial infection of the tissue and bone surrounding the implant, functionally equivalent to periodontitis around natural teeth
- Chronic parafunctional habits such as bruxism (tooth grinding) without occlusal protection
- Inadequate long-term oral hygiene and absence of regular professional maintenance
How risk is mitigated at a high-standard clinic:
- 3D CBCT scanning identifies bone volume and density deficienciesbefore surgery
- Computer-guided surgical templates eliminate technique-dependent placement errors
- Strict two-stage protocols prevent premature loading
- Patient education on long-term hygiene and maintenance reduces peri-implantitis risk
- Premium implant brands (Straumann, Nobel Biocare) utilise surface technologies specifically engineered to reduce bacterial adhesion and support healthier peri-implant tissue
Dental Implants vs. Dentures vs. Bridges: Which Is the Better?
Dental implants are superior. From a clinical and biological standpoint, this is unambiguous. The comparison below reflects documented differences in biological outcome, structural impact on adjacent teeth, and long-term longevity.
Dentures | Bridge | Implant | |
Replaces the tooth root | ✗ No | ✗ No | ✓ Yes |
Preserves jawbone | ✗ No | ✗ Partial | ✓ Yes |
Impact on adjacent teeth | ✗ stress neighbouring teeth | ✗ Grinding downs healthy teeth | ✓ Fully independent |
Chewing (vs. Natural function) | ~25% | ~70–80% | ~95–100% |
Longevity | 5–8 years | 10–15 years | 20-25 years |
FAQs
What is the 3/2 rule for dental implants?
The 3/2 rule is a safety guideline for bone margin around the implant fixture. It requires a minimum of 3 mm of bone above the tip of the implant and 2 mm of bone laterally (to either side). These margins ensure the implant has sufficient surrounding bone for stable osseointegration and reduce the risk of bone dehiscence.
Are you asleep when they do dental implants?
You are awake but fully numb. Implant surgery is performed under local anaesthesia, which eliminates all pain while keeping you conscious. General anaesthesia (being fully asleep) is not required and is generally reserved for highly complex full-arch cases or patients with severe dental phobia.
What is the downside of having dental implants?
The main drawbacks are the cost, the surgery, and the healing time. Specifically:
- Thetotal process takes 4–7 months
- The procedure involvesminor oral surgery
- Implants are asignificant financial investment
- Patients who smoke, have uncontrolled diabetes, or have severe bone loss require additional preparatory treatment
How many teeth can be fixed on one implant?
One implant typically supports one crown. However, a single implant can support more than one tooth:
- Implant-supported bridgesuse two implants to support three teeth (one pontic in the centre)
- All-on-4 and All-on-6 systems use four or six implants respectively to support a full arch of 10–12 teeth
What is the most painful part of a dental implant?
The most uncomfortable phase is the post-op recovery, not the surgery itself. Once the local anaesthesia wears off 3–5 hours after the procedure, patients experience swelling and soreness on day 1 and day 2. This is manageable with prescribed medication and ice.
Which is worse, tooth extraction or implant?
For most patients, a tooth extraction is more uncomfortable than implants. Extractions can involve significant pressure and post-op soreness. Implants are placed on healthy bone with a guided drill and produce less trauma.
What I wish I knew before dental implants?
The most common things patients say they wish they had known:
- The procedure is far less painful than expected
- Verification of implant brand is your right— always ask for the original manufacturer packaging with REF and LOT codes
- The process takes months, not days
- Temporary crowns are not the final result
- Bone grafting may be needed
- Smoking genuinely threatens the result
Which is healthier, a root canal or an implant?
A dental implant is considered healthier when the natural tooth cannot be saved. A root canal preserves the natural tooth root, which is always preferred. However, when a tooth or its roots deteriorate, risks often outweigh the benefits of an implant.
Can I drive myself home after dental implant surgery?
Yes, but only if you received local anaesthesia. Local anaesthesia affects only the numb area and does not impair cognition, coordination, or reaction time once the injection procedure is complete. If you received conscious sedation or intravenous sedation, you must not drive for a minimum of 24 hours.
How painful is tooth extraction on a scale of 1 to 10?
During the procedure: 1–2 out of 10. Post-operatively: 3–5 out of 10, peaking within the first 24–48 hours. More complex cases such as impacted wisdom teeth, fractured roots, or infected teeth, may reach 5–6 out of 10 in the first 48 hours.