Early implant failure symptoms are often subtle at first: a dull ache that won’t go away, slight movement, or gums that look inflamed. Many patients dismiss these signs as normal post-op. Great mistake. Recognizing the early signs of dental implant failure gives you the best possible chance of saving the implant — and avoiding more complex, expensive treatment.
This guide walks you through everything you need to know, from the first warning signals to the risk factors that make failure more likely.
What Factors Impact Dental Implant Success?
Dental implants are one of the most reliable, long-lasting solutions for missing teeth. With success rates exceeding 95% over ten years. Yet, like any surgery, they carry risks.
Several key factors determine whether a dental implant will succeed: the quality and density of your jawbone, your overall health, the surgical technique, and how carefully you follow post-operative care instructions. When any of these elements are compromised, the dental implant failure may occur — either early, during the healing phase, or later, after years of function.
What Is Early Dental Implant Failure?
Early dental implant failure is the loss or rejection of an implant before the final prosthesis is placed — typically within the first three to four months after surgery. This is the window during which the implant must fuse with the jawbone through osseointegration. If that fusion fails, the implant fails.
Early implant failure is linked to biological problems where the body does not properly accept the implant. It may be connected to immunological, genetic, and systemic variables.
It is important to distinguish early failure from late failure, which occurs months or years after successful integration — usually due to infection or mechanical overload. Early failure is different: it happens during healing, before the implant ever has a chance to function.
What Causes Early Dental Implant Failure?
The main causes of early implant failure include excessive heating of the bone during drilling, over-preparation of the surgical site, and low bone density — all of which interfere with the stability of the implant.
Beyond surgical factors, systemic and biological causes play a major role:
- Failed osseointegration. Early failures occur due to the inability to establish close contact between bone and implant, absence of bone apposition, and formation of fibrous tissue between the implant surface and surrounding bone.
- Systemic disease. Uncontrolled diabetes, osteoporosis, cardiovascular disease, and smoking all impair healing and increase failure risk significantly.
- Implant overload. Placing functional pressure on an implant before osseointegration is complete can disrupt the bonding process entirely.
- Surgical error. Research confirms that the seniority of the surgeon has a statistically significant effect on early implant failure — with less experienced operators carrying a nearly threefold higher adjusted risk.
- Improper implant positioning. Incorrect angulation or depth affects both stability and long-term prosthetic outcomes.
First Stage: The Critical Osseointegration Window
Osseointegration typically takes 3 to 6 months to complete. During this time, bone cells grow directly onto the implant surface, creating a strong mechanical bond. Without successful osseointegration, the implant will remain loose and eventually fail.
This is the most vulnerable phase of the entire implant process. Any disruption — bacterial infection, excessive pressure, poor bone density, or compromised healing — can prevent the bone from bonding correctly with the titanium post.
The two major mechanisms responsible for failure during this stage are infection and impaired healing. Bacterial infection can occur at any point during treatment, but is especially dangerous during the early healing period. This is why post-operative care and antibiotic protocols are not optional — they are critical.
7 Early Implant Failure Symptoms to Watch For
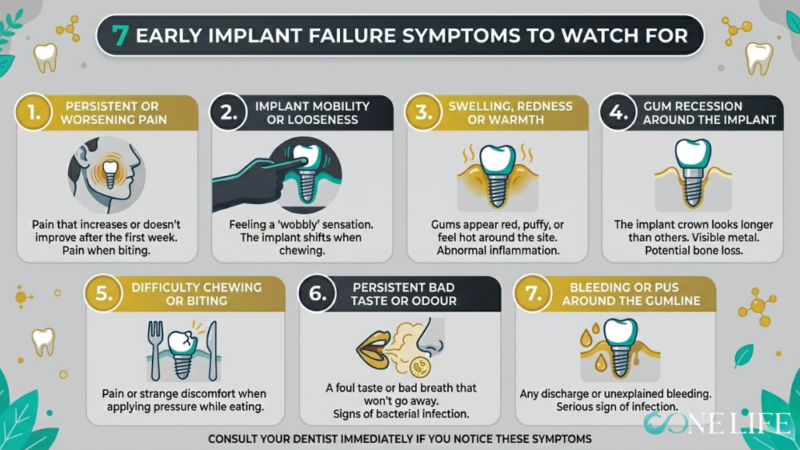
If you notice persistent pain, a loose implant, swelling around the gums, or difficulty chewing, these could be signs your dental implant is failing. Many patients assume some discomfort is normal and wait too long to get help — but ignoring these symptoms can lead to infection, bone loss, and the need to remove the implant entirely.
Here are the seven warning signs to take seriously:
- 1. Persistent or worsening pain. Some discomfort after surgery is expected. But pain that worsens instead of improving, sharp or throbbing sensations weeks after placement, or pain triggered by biting down are all warning signs that something is wrong.
- 2. Implant mobility or looseness. Mobility is often the first sign of a failing implant. Initially there may be only very slight movement — recognizable only to a dentist — but over time a failing implant will feel wobbly and may shift when chewing or talking.
- 3. Swelling, redness or warmth. Swelling, redness, or warmth at the implant site signals inflammation or infection. This is abnormal and requires immediate attention from your dentist.
- 4. Gum recession around the implant. If the implant crown appears longer than surrounding teeth, or the metal post becomes visible above the gumline, gum recession is occurring — a sign of potential bone deterioration.
- 5. Difficulty chewing or biting. Pain or discomfort when chewing or biting on the implant indicates that integration between the implant and bone has not occurred correctly.
- 6. Persistent bad taste or odour. A persistent bad taste or foul odour can indicate bacterial infection, poor hygiene, or failure in infection control around the implant site.
- 7. Bleeding or pus around the gumline. Any discharge or unexplained bleeding around the implant post is a red flag that should never be ignored. Contact your dental team immediately.
What To Do If You Notice These Symptoms
Do not wait. The difference between catching a problem at week two versus month six can determine whether your implant survives or requires complete removal and replacement.
If you experience any of the symptoms described above, follow these steps immediately:
- Contact your dental clinic the same day — do not wait for your next scheduled appointment
- Do not apply pressure to the implant area — avoid hard foods and aggressive brushing around the site
- Document your symptoms — note when they started, how they have changed, and any factors that worsen them
- Bring a full list of your medications to your appointment — some drugs directly affect healing
- Request an X-ray — peri-implant bone loss is only visible radiographically and must be assessed professionally
Risk Factors at a Glance
The following table summarizes the most significant risk factors for early dental implant failure, based on peer-reviewed research:
Risk Factor | Impact on Failure Risk | Notes |
High | Impairs blood supply and healing | |
Uncontrolled diabetes | High | Slows osseointegration |
Poor bone density | High | Reduces primary implant stability |
Bacterial infection | High | Leading cause during healing phase |
Inexperienced surgeon | Moderate–High | Studies show residents have up to 2.86x higher failure risk |
Maxillary (upper jaw) placement | Moderate | 83% of lost implants in one study were in the upper jaw |
Certain medications | Moderate | Including heartburn drugs, immunosuppressants |
Autoimmune conditions | Moderate | Rheumatoid arthritis, osteoporosis |
Bruxism (teeth grinding) | Moderate | Places excessive load on healing implant |
Poor post-op hygiene | Moderate | Increases infection risk significantly |
Preventing Dental Implant Failure
Prevention starts before the surgery, not after. A thorough pre-operative assessment — including bone density scans, full medical history review, and risk factor screening — is the foundation of a successful implant outcome.
Key prevention strategies include:
- Quitting smoking at least 2 weeks before surgery and throughout healing
- Controlling systemic conditions such as diabetes before the procedure
- Following all post-operative hygiene instructions without exception
- Attending every follow-up appointment, even when you feel fine
- Avoiding hard foods and excessive bite pressure during the osseointegration phase
- Disclosing all medications to your surgeon, including over-the-counter drugs
Certain medications, including common heartburn drugs, have been shown to reduce new bone growth — potentially affecting how an implant fuses with the jawbone. Your surgical team needs the full picture to keep you safe.
What is the Success Rate of Dental Implants in Turkey?
Turkey has become one of the leading destinations in the world for dental implant treatment, combining internationally trained specialists, state-of-the-art facilities, and significantly lower costs than Western Europe or North America — without compromising on clinical standards.
Large-scale studies show dental implant survival rates of over 96% at five years — and clinics in Turkey operating at the highest level consistently meet or exceed these benchmarks. The key differentiator is not geography, but the experience of the surgical team, the quality of the implant system used, and the rigor of pre-operative planning.
Dental implants in Turkey begins with a comprehensive 3D CBCT scan, a full medical and pharmacological assessment, and a personalized treatment plan tailored to your bone structure and health profile. Our protocols are designed to minimize the risk of early failure at every stage — from patient selection through to long-term follow-up.
FAQ’s
What is the most common symptom of early dental implant failure?
Implant mobility — any detectable movement of the implant post — is the clearest clinical indicator of early failure. It signals that osseointegration has not occurred correctly.
How soon after surgery can early failure occur?
Early failure typically happens within the first 3 to 4 months after placement, during the osseointegration window when the jawbone needs to fuse with the implant.
Can early dental implant failure be treated?
In some cases, yes. If caught very early, infection can be treated and the implant stabilized. In other cases, the implant must be removed, the site allowed to heal, and a new implant placed after several months.
How common is early dental implant failure?
Early failure rates for dental implants are around 1–2% at the implant level. At the patient level, approximately 3% of people lose at least one implant in the upper jaw during the first year.
Does smoking significantly increase failure risk?
Yes. Smoking impairs blood circulation and immune response, both of which are essential for healthy osseointegration. It is one of the most consistently cited modifiable risk factors in the clinical literature.
Is pain after implant surgery always a warning sign?
Not immediately. Some discomfort in the first few days is normal. The concern is pain that worsens over time, persists beyond two weeks, or is triggered by biting and chewing — those patterns warrant urgent evaluation.
Can I get a replacement implant after early failure?
In most cases, yes — once the site has fully healed and any underlying risk factors have been addressed. Your surgeon will reassess bone volume and systemic health before proceeding.