Dental implants are expensive, which begs the question: will they actually work? The answer is backed by decades of research and clinical practice. Dental implants are the most predictable tooth replacement solution in modern dentistry, with success rates that exceed 95% in healthy patients. But what do those numbers really mean, and what determines whether your implant succeeds or fails?
What Is a Dental Implant and How Does It Work?

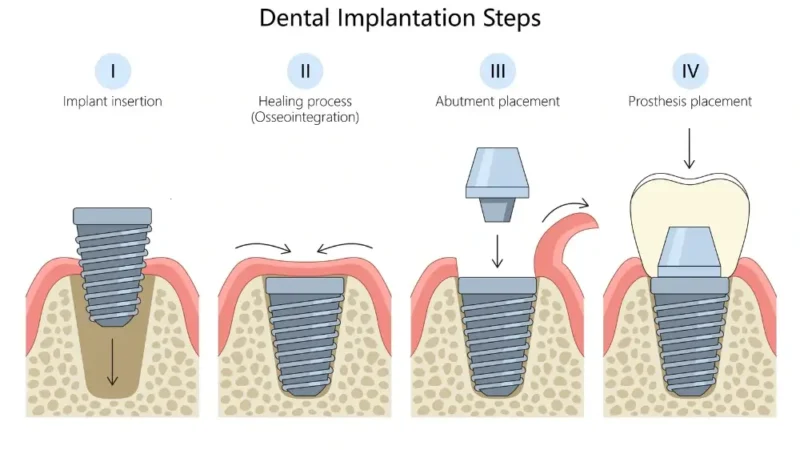
A dental implant is a small titanium screw that replaces the root of a missing tooth. Once inserted, it fuses with the surrounding bone and becomes a stable, permanent anchor for a crown, bridge, or full arch of teeth. Titanium is used because it is biocompatible: the body does not reject it. The result is a tooth that looks, feels, and functions like a natural one.
What Is the Success Rate of Dental Implants?
Dental implants succeed in 95% to 98% of cases according to peer-reviewed clinical research. The global average failure rate for dental implants is 3.1% Impressions Dental, while specific systems perform even better: the survival rate of All-on-4 dental implants reaches 98.8% Impressions Dental.
It is worth distinguishing between survival rate (the implant is still in place) and success rate (the implant is in place and functioning without complications). Success is the higher bar — and implants still clear it with exceptional consistency.
Here is a quick summary of what the numbers look like:
- Single implant success rate (10 years): 2%
- All-on-4 cumulative survival rate: 8%
- Global implant failure rate: ~3.1%
- Implants with bone grafting success rate: 83%
- Long-term success (25+ years with proper care): 80% documented and achievable
Dental Implant Success After 10 and 20 Years
Will implants still be working after decades? The research on this is extensive. Data published in the Journal of Clinical Periodontology shows an overall 10-year success rate of 95.2%. The long-term picture is equally compelling with 88-92% survival after 20 years. Springer
These figures are strong — but long-term success is not automatic. It is earned through good oral hygiene, professional maintenance, and avoiding key risk behaviours such as smoking.
Time Period | Approximate Survival Rate |
1 year | ~98–99% |
5 years | ~97% |
10 years | ~95–96% |
20 years | ~88–92% |
38–40 years | ~95.6% (landmark Brånemark study) |
What Factors Affect the Success Rate of Dental Implants?
Implant success is the result of multiple variables working together. For example, age, health conditions, smoking status, and prosthetic design significantly influence implant survival. Below, we break the most important factors down.
- Bone quality and quantity: The implant needs sufficient dense bone to anchor into. Patients with significant bone loss may require a bone graft before implant placement.
- Implant location: Implants placed in the lower jaw (mandible) tend to have slightly higher success rates than those in the upper jaw (maxilla).
- Surgeon experience and technology: The skill and experience of the implantologist matters enormously. Clinics using CBCT 3D imaging, computer-guided surgery, and premium implant brands — such as Nobel Biocare or Straumann — consistently report better outcomes.
- Oral hygiene: Implants cannot decay, but the gum and bone around them can become infected — a condition called peri-implantitis. Poor oral hygiene is one of the leading causes of late implant failure.
- Systemic health: Conditions such as uncontrolled diabetes, autoimmune disorders, and osteoporosis can impair healing and osseointegration.
Here is a summary of the main factors and their impact:
Factor | Impact on Success Rate |
Adequate bone volume | High — foundation of osseointegration |
Surgeon experience & technology | High — directly affects placement precision |
Oral hygiene post-treatment | High — prevents peri-implantitis |
Smoking | High negative impact (see next section) |
Uncontrolled diabetes | Moderate to high negative impact |
Implant location (upper vs lower jaw) | Moderate — upper jaw slightly lower rates |
Implant brand & surface technology | Moderate — premium brands show better data |
Smoking, Diabetes and Other Risk Factors
Knowing what specifically could affect your dental implant result is what truly matters. Some risk factors are fixed; others are entirely within your control. Here is an honest breakdown.
Smoking: The Single Biggest Risk
Nicotine constricts blood vessels, reducing oxygen supply to healing tissues and dramatically slowing osseointegration. The numbers are stark. Smokers face implant failure rates roughly two to three times higher than non-smokers. The risk is dose-dependent — heavier smokers fare worse — and it does not disappear after placement.
Diabetes
Uncontrolled diabetes impairs immune response and slows tissue healing, both of which are critical in the weeks following implant surgery. However, diabetes alone is not a contraindication. Patients with well-controlled blood sugar levels consistently achieve success rates comparable to non-diabetic patients. The key is coordination between your implant surgeon and your physician to ensure your HbA1c levels are optimised before treatment begins.
Other Risk Factors Worth Knowing
Beyond smoking and diabetes, the following conditions and behaviours can influence outcomes:
- Osteoporosis and bisphosphonate medication— these drugs, used to treat bone density loss, can interfere with jawbone healing and require specialist assessment before implant surgery
- Autoimmune conditions— diseases such as lupus or rheumatoid arthritis may affect healing; each case must be evaluated individually
- Bruxism (teeth grinding)— excessive grinding places abnormal mechanical stress on implants, increasing the risk of crown fracture or implant failure over time; a custom night guard is often recommended
- Poor oral hygiene— as noted, peri-implantitis is a leading cause of late failure and is largely preventable with consistent home care and professional maintenance
- Alcohol consumption— heavy alcohol use impairs bone metabolism and immune function, increasing early failure risk
Are Dental Implants in Turkey as Successful as in the UK or US?
Yes, dental implants in Turkey can achieve the same success rates as in the UK or US — provided you choose the right clinic. Turkey has become one of the world’s leading destinations for implant dentistry, and the numbers reflect genuine clinical infrastructure. The key indicators to look for are:
- Premium implant brands— leading clinics use the same systems as UK and US surgeons: Nobel Biocare, Straumann, and equivalent internationally certified brands
- CBCT 3D imaging— essential for accurate pre-surgical planning and anatomical assessment
- Specialist surgeons— look for oral and maxillofacial surgeons or periodontists, not general dentists performing implant surgery
- International accreditation— certifications such as ISO 9001, JCI, or membership of recognised dental bodies signal adherence to clinical standards
- Transparent guarantees— reputable clinics provide written warranties on both the implant and the prosthetic crown
How to Maximise Your Dental Implant Success Rate
There are concrete steps you can take, before and after treatment, to push your dental implant success rate as close to 100% as possible. Think of it as a partnership between you and your surgical team.
Before Treatment
What you do in the weeks leading up to surgery matters more than most patients realise. The following steps meaningfully improve outcomes:
- Stop smoking at least two weeks before surgery, and ideally longer
- Optimise blood sugar if you have diabetes — work with your physician to bring HbA1c to a safe level before the procedure
- Complete a thorough dental assessment— CBCT 3D imaging should be standard
- Address active gum disease — any existing infection in the mouth must be treated and resolved before implant placement
- Discuss all medications with your surgeon
During Treatment
Individual success depends on many factors, including the quality and amount of jawbone and the skill of the dentist performing the procedure. Verify that your surgeon is a specialist — not a general dentist — and that the clinic uses a premium, internationally certified implant system with verifiable REF and lot codes.
After Treatment
During the healing phase, follow these guidelines rigorously:
- Do not smoke during the healing period — this is non-negotiable
- Eat soft foods for the first weeks post-surgery
- Maintain oral hygiene — gentle brushing around the implant site, interdental brushes, and antibacterial mouthwash as directed
- Attend all follow-up appointments — your surgeon needs to monitor bone integration, gum health, and crown fit at regular intervals
- Wear a night guard if you grind your teeth
Long-Term Maintenance
Implants can keep you smiling for at least 25 years when installed correctly and properly maintained — but they need daily brushing and flossing, and regular professional visits to check surrounding tissue and bone. A professional clean every six months, combined with annual radiographic monitoring of bone levels, is the minimum standard for long-term implant health.
FAQs
What is the success rate of dental implants?
Dental implants are highly reliable, with success rates that range from 90% to 98%, and long-term success extending beyond 25 years with proper care. In healthy, non-smoking patients with good bone volume, results consistently sit at the higher end of that range.
What is the dental implant success rate after 20 years?
A 2024 analysis published in Clinical Oral Investigations found a mean survival rate of 92% at 20 years, with retrospective studies showing 88%. These figures reflect older implant systems; implants placed today with modern surface technology are expected to perform better.
What is the success rate of dental implants in older patients?
Older patients can achieve excellent outcomes provided good bone density and health. Late implant failures are associated with bone quality in older adults — which is why thorough pre-surgical assessment, including CBCT imaging, is especially important for patients over 65.
Do dental implants fail often?
No. The global average failure rate for dental implants is 3.1% — meaning the overwhelming majority of implants placed worldwide integrate successfully and remain functional long-term. Most failures occur within the first few months, during osseointegration, and are typically correctable with a replacement implant.
Does smoking really affect dental implant success?
Yes — significantly. Smoking is the single most impactful modifiable risk factor for implant failure. It restricts blood flow to healing tissues, slows osseointegration, and increases the risk of peri-implantitis. Smokers face failure rates roughly two to three times higher than non-smokers. Stopping before and during the healing phase materially improves outcomes.
What can I do to improve my implant success rate?
The most impactful steps are: stop smoking, optimise systemic health before surgery, choose a specialist implantologist using premium implants and 3D imaging, maintain rigorous oral hygiene post-treatment, and attend all follow-up appointments. Long-term success is a shared responsibility between patient and clinician.

