Many patients believe that a lack of jawbone density disqualifies them from receiving permanent tooth replacements. However, clinical advancements in restorative dentistry have made it possible: No bone, no problem!
When a natural tooth is lost, the alveolar bone—the part of the jawbone that supports teeth—no longer receives the stimulation required for bone remodeling. Within the first year of tooth loss, studies indicate a 25% decrease in bone volume in the affected area. This process, known as atrophy, continues over time, leading to a thinner and shorter jaw ridge that complicates traditional implant placement.
Common Causes of Dental Bone Loss
While the primary driver of jawbone depletion is tooth extraction without replacement, several other medical and lifestyle factors contribute to decreased bone density. Identifying the root cause is essential for your surgeon to determine the most effective reconstructive strategy that suits your needs.
- Tooth Loss (Anodontia/Extraction): When a tooth is removed, the surrounding alveolar bone loses its function. Without the tooth root to provide mechanical stress, the body begins to reabsorb the bone tissue.
- Periodontal Disease: Chronic gum infections destroy the attachment fibers and supporting bone that hold teeth in place.
- Long-term Denture Use: Traditional dentures do not stimulate the bone; in fact, the friction and pressure can accelerate bone resorption.
- Physical Trauma: A forceful blow to the jaw can cause bone fragments to die or teeth to be knocked out, leading to localized bone loss.
- Systemic Health Conditions: Conditions like osteoporosis or uncontrolled diabetes can interfere with the body’s ability to maintain or heal bone tissue.
Indications of Bone Loss
Recognizing the signs of bone resorption early simplifies the treatment plan. If you have been missing teeth for several years, it is highly likely that some degree of bone loss has occurred. Evaluation via CBCT (Cone Beam Computed Tomography) scans is the gold standard for diagnosis, but patients often notice physical changes first.
Common indicators include:
- A visible recession of the gum line,
- Shifting of the remaining natural teeth
- Change in the way your dentures fit
- Distance between nose and chin decrease, creating deep wrinkles around the mouth (in advanced cases)
If you experience these symptoms, a bone density assessment is required before proceeding with dental implant surgery.
How Much Bone is needed for Dental Implants?
For a dental implant to last a long time, it must be surrounded by a specific volume of healthy bone. This ensures primary stability during the initial placement and allows for osseointegration—the biological process where the bone fuses with the titanium post. Surgeons typically look for a minimum of 1mm to 2mm of bone thickness around the circumference of the implant.
Solutions: Bone Grafting and Sinus Lifts
Surgeons utilize bone augmentation to “build” the jaw back to its original dimensions. These procedures are highly routine and are often performed under local anesthesia or sedation to ensure patient comfort.
The most common solutions include Guided Bone Regeneration (GBR) and Sinus Lifts. By placing specialized grafting material into the deficient site, the surgeon creates a scaffold that encourages your body to grow a new bone. Over a period of 4 to 9 months, this material is replaced by natural bone tissue, providing an anchor for future implants.
Comparison of Bone Restoration Solutions
Procedure | Target Area | Purpose | Recovery Time (Healing) |
Socket Graft | Extraction Site | Prevents bone collapse after losing a tooth | 3 – 4 Months |
Lateral Ridge Augmentation | Jaw Ridge | Increases the width/thickness of the jawbone | 4 – 6 Months |
Sinus Lift | Upper Posterior | Raises the sinus floor to add vertical height | 6 – 9 Months |
Block Bone Graft | Large Deficiencies | Uses a “block” of bone for significant volume loss | 6+ Months |
Socket Graft (Socket Preservation)
Performed immediately following a tooth extraction where grafting material is placed into the empty socket to prevent bone collapse and preserve the surrounding ridge.
Procedure: After tooth removal, the dentist fills the socket with bone graft material (synthetic, cadaver, or bovine bone), often covering it with a membrane to promote healing.
Goal: To prevent the natural 40-60% loss in ridge width/height that occurs within 6-12 months after extraction, which can make future implants difficult.
Benefits: It maintains facial aesthetics, improves the success rate of future implants, and ensures there is enough bone for a stable, long-lasting restoration.
Lateral Ridge Augmentation
Surgical procedure often performed by periodontists, that increases the width of the jawbone to create a stable foundation for dental implants. It involves using bone grafts or substitutes to repair areas with significant bone loss, typically after tooth extraction. This procedure enables successful implant placement even in cases of narrow or resorbed alveolar ridges.
Procedure: The most common method is Guided Bone Regeneration (GBR), which uses bone substitutes and barrier membranes to promote bone growth
Goals: When performed by a professional, the success rate is over 90%. Patients may experience pain for about 3 days after the procedure.
Benefits: This procedure helps to prevent facial collapse that often follows tooth loss and provides a better foundation for the long-term health of dental implants.
Sinus Lift
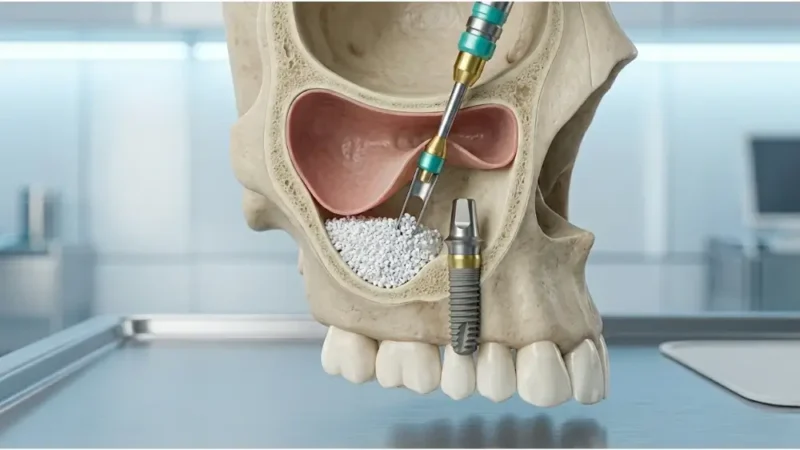
When there is insufficient height in the upper jaw due to sinus pneumatization, a sinus lift is required. This procedure pushes the sinus membrane upward to make room for new bone.
Procedure: The surgeon gently lifts the sinus membrane and places grafting material into the space between the jawbone and the sinus cavity.
Goals: The primary goal is to increase vertical bone height in the upper posterior jaw to safely accommodate dental implants.
Benefits: This procedure successfully restores implant viability in areas previously limited by sinus proximity.
Types:
- Internal Sinus Lift (Osteotome Technique): Used when only a small amount of bone is needed. The lift is performed through the same hole created for the implant.
- Lateral Window Sinus Lift: Used for more significant bone loss. A small “window” is created in the side of the jaw to access the sinus cavity and place a larger volume of grafting material.
Block Bone Graft
Designed to repair significant jawbone loss or structural defects. By attaching a solid piece of bone—either from the patient’s own body (or an animal source (xenogenic)—to the jaw ridge using small titanium screws, surgeons can create a stable foundation for future dental implants.
This method is often preferred for severe cases as it provides superior volume and shape retention compared to using loose, particulate bone granules.
Procedure: A solid block of bone is harvested or sourced and secured to the deficient area of the jaw using titanium screws to provide a structural scaffold.
Goals: This technique aims to reconstruct significant horizontal or vertical bone deficiencies to create a dense, stable foundation for multiple implants.
Benefits: Block grafting provides superior structural integrity for severe bone loss cases, allowing for natural bone integration and improved long-term aesthetic results.
Types of Bone Graft Materials
The choice of grafting material depends on the extent of the bone resorption and the patient’s medical history. Modern dentistry offers several biocompatible options, each with specific advantages for osteogenesis (new bone growth).
- Autografts: Bone taken from the patient’s own body (usually the chin or hip). It is the gold standard for biocompatibility.
- Allografts: Processed human bone from a certified tissue bank. It is highly effective and eliminates the need for a second surgical site.
- Xenografts: Bone derived from another species, typically bovine. These provide an excellent calcium scaffold for human bone to grow into.
- Alloplasts: Synthetic materials, such as hydroxyapatite or calcium phosphate, used to stimulate natural bone repair.
Zygomatic and All-on-4 Implants for Severe Bone Loss
In cases of extreme maxillary bone resorption where traditional grafting may be too invasive or lengthy, advanced surgical alternatives like Zygomatic implants offer a solution. Unlike standard implants that anchor into the jawbone, Zygomatic implants are longer and anchor into the zygoma (cheekbone). This bone is extremely dense and does not resorb like the jawbone, providing an extremely stable foundation.
For patients with moderate bone loss, the All-on-4® treatment concept utilizes tilted posterior implants to maximize the use of available bone. By angling the implants at 45 degrees, surgeons can often avoid the need for sinus lifts or extensive grafting, making the recovery time much shorter.
Success Rates and Medical Statistics
Clinical data confirms that bone loss does not have to compromise the longevity of your dental restoration. According to the International Journal of Implant Dentistry, the success rate for implants placed in grafted bone is remarkably high, often exceeding 95% over a ten-year period.
- 98% Success Rate: For standard implants in healthy bone.
- 94% – 97% Success Rate: For implants placed following a sinus lift or ridge augmentation.
- 92% Success Rate: For Zygomatic implants in patients with severe upper jaw atrophy.
Step-by-Step: The Dental Implant Procedure with Preliminary Grafting
The journey to a restored smile when dealing with bone loss typically follows a structured, multi-phase medical protocol to ensure the highest safety and aesthetic outcome.
- Consultation and 3D Imaging: Utilizing CBCT scans to map bone volume and nerve locations.
- Bone Augmentation: The grafting material is placed. Depending on the technique, this may be done simultaneously with the implant or as a separate stage.
- Healing Phase (Osseointegration): A period of 3 to 6 months where the graft matures and the implant fuses with the bone.
- Abutment Placement: A small connector is attached to the implant post.
- Final Restoration: Your custom-made dental crown or bridge is securely attached.
Recovery Time and Essential Aftercare Tips
Recovery from bone grafting and implant surgery is generally manageable with standard post-operative care. Most patients return to work within 2 to 3 days, although the healing of the bone continues for several months.
- Soft Food Diet: Avoid hard or crunchy foods for the first 2 weeks to prevent pressure on the surgical site.
- Oral Hygiene: Use a prescribed antimicrobial mouthwash and avoid brushing directly on the stitches for the first few days.
- No Smoking: Tobacco use significantly restricts blood flow to the bone, increasing the risk of graft failure by over 30%.
Frequently Asked Questions (FAQs)
Is bone grafting for dental implants painful?
The procedure is performed under local anesthesia or sedation. Most patients report only mild discomfort and swelling post-surgery, which is easily managed with prescribed analgesics.
How long do I have to wait for an implant after a bone graft?
It typically takes 4 to 6 months for a bone graft to fully integrate and become strong enough to support an implant, though some “immediate load” cases allow for faster timelines.
Can my body reject a bone graft?
While rare, “rejection” usually refers to the graft failing to integrate. This is often caused by infection or smoking rather than an immune response, especially with biocompatible materials.
How long does a bone graft last?
Once a bone graft has successfully integrated with your natural jawbone, it becomes a permanent part of your anatomy. With proper oral hygiene and regular dental checkups, the graft is designed to last a lifetime, providing the long-term foundation needed for your dental implants.

