Losing a tooth is never just a cosmetic issue. For people with diabetes, it can be the start of a cycle that affects nutrition, metabolic control, and overall health. The good news: dental implants for diabetic patients are not off-limits. But the outcome depends on factors that need to be understood before treatment begins. Poorly managed diabetes can compromise the longevity of dental implants and increase the risk of failure.
Why Diabetes and Tooth Loss Are More Connected Than You Think
The relationship between diabetes and oral health is bidirectional. Poor blood sugar accelerates gum disease and tooth loss — and tooth loss, in turn, can limit the ability to eat a nutritious, balanced diet. After tooth loss, patients tend to avoid foods that require more effort to chew, which can lead to poor nutrition and reduced metabolic control.
Diabetes also causes chronic inflammation in the mouth. High blood sugar levels can lead to dry mouth, which raises the risk of cavities and gum disease, while the inflammation makes it easier for bacteria to thrive, leading to more severe periodontal issues.
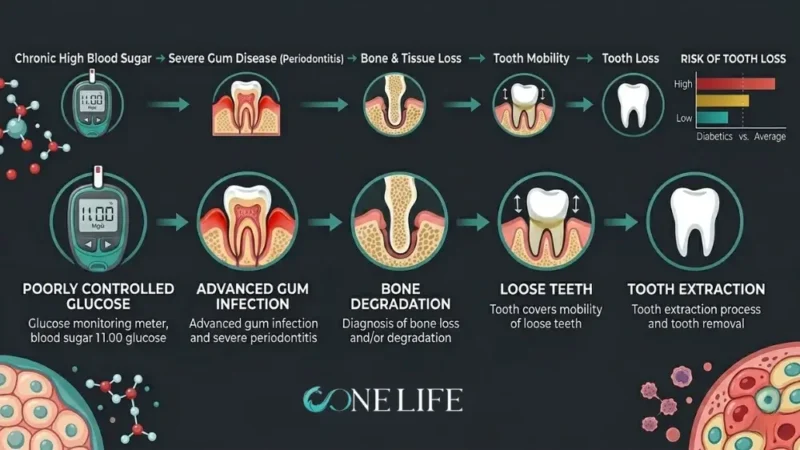
How Diabetes Affects Dental Implant Osseointegration
Osseointegration — the process of dental implants fusing with jawbone — is the biological foundation of implant success. In diabetic patients, this process faces specific challenges. Hyperglycemia worsens bone mineral density and triggers a proinflammatory state that reduces insulin-like growth factor 1 (IGF-1) levels, impairing both bone matrix synthesis and bone formation. The result is slower, less predictable healing during the critical weeks after implant placement.
Diabetic patients face higher risks of peri-implantitis and compromised osseointegration due to the adverse effects of diabetes on bone metabolism and immune response. However, these risks are significantly modifiable — and that distinction matters enormously for treatment planning.
The Role of HbA1c & Glycemic Control
HbA1c (glycated haemoglobin) measures average blood glucose over the preceding 2–3 months. It is the most important predictor of implant outcomes in diabetic patients. Clinically, the thresholds are clear:
- HbA1c ≤ 8% → Well-controlled: implant outcomes comparable to non-diabetic patients
- HbA1c 8.1–10% → Moderately controlled: elevated risk, requires careful protocol
- HbA1c > 10% → Poorly controlled: significantly impaired osseointegration and higher failure risk
When diabetes is well-managed (HbA1c below 8%), it does not significantly compromise implant survival rates, with survival percentages ranging from 96.1% to 97.3% at one year and 87.3% to 96.1% at five years, comparable to non-diabetic populations.
Patients with lower glycemic control show a lower implant stability quotient (ISQ) in the period of 2–12 weeks post-placement — and the lower the level of glycemic control, the longer the recovery to baseline stability takes. Most implants, however, reach baseline stability within four months even in moderately uncontrolled patients, provided there are no micro- or macro-vascular complications.
Controlled vs. Uncontrolled Diabetes for Dental Implants
The contrast between well-managed and poorly managed diabetes in implant outcomes is striking. A study involving 41 patients with well-controlled Type 2 diabetes showed a success rate of 97.2% at one year and 94.4% at five years.
By contrast, poorly controlled diabetes (HbA1c above 8%) adversely affects peri-implant health metrics, including marginal bone loss and probing depth, with outcomes worsening progressively as HbA1c levels increase. PubMed In patients with HbA1c between 8.0 and 8.9%, the implant failure rate reaches approximately 9%, and survival drops further as glycemic control deteriorates — with patients in the 11.0–11.9% HbA1c range recording a survival rate of only 75%. Glycemic control before surgery is not optional — it is the single most important predictor of long-term implant success in diabetic patients.
Risks of Peri-Implantitis in Diabetic Patients
Peri-implantitis — inflammation of the tissue surrounding an implant — is the leading cause of late implant failure. Diabetes amplifies this risk considerably.
Studies show that diabetic patients are 1.9 to 4.1 times more likely to develop peri-implantitis than non-diabetic patients — meaning the risk is roughly double to quadruple depending on the duration of follow-up and level of glycemic control — and this risk increases progressively as HbA1c values rise.
Key mechanisms behind this risk include:
- Impaired immune response: reduced ability to fight bacterial infection around the implant
- Delayed wound healing: slower soft tissue closure increases the infection window post-surgery
- Chronic inflammation: systemic inflammatory markers remain elevated, affecting peri-implant tissues
- Reduced collagen repair: diabetic patients produce more glycosylation end-products that lead to collagen cross-linking, reducing the likelihood of collagen repair and replacement in periodontal and peri-implant tissues
Peri-implantitis risk in diabetic patients is real but manageable through strict oral hygiene, regular monitoring, and appropriate pharmacological support.
Dental Implant Success Rates: What the Numbers Show
Glycemic Control Level | HbA1c Range | Implant Survival at 1 Year | Implant Survival at 5 Years | Key Risk |
Well-controlled | < 8% | 96.1% – 97.3% | 87.3% – 96.1% | Minimal |
Moderately controlled | 8.1% – 10% | ~90–93% | ~80–88% | Elevated peri-implantitis risk |
Poorly controlled | > 10% | Significantly reduced | Significantly reduced | High failure & bone loss risk |
Non-diabetic (reference) | N/A | ~97–98% | ~94–96% | Baseline |
Sources: PubMed systematic reviews (2022–2024), Cureus, Frontiers in Pharmacology
Are you a Candidate for Dental Implants with Diabetes?
Not every diabetic patient is an identical candidate, but the vast majority of well-managed patients qualify. The key is not whether you have diabetes — it is how well it is controlled and how thoroughly the pre-surgical assessment is conducted. A skilled implant specialist will never make a decision based on diagnosis alone. The assessment must be individualized, multidisciplinary, and thorough.
It is also worth reframing the question entirely. Rather than asking “can I get implants despite my diabetes?”, the more productive question is: “what needs to be in place for my implants to succeed?” In most cases, the answer is achievable with the right preparation and the right team.
Pre-Surgical Requirements and Assessment
Before proceeding with implant placement, your dental specialist should conduct a comprehensive evaluation that includes:
- HbA1c measurement: ideally below 8% before surgery is scheduled
- Full periodontal assessment: any existing gum disease must be treated and stabilized first
- Bone density evaluation: via CBCT (cone beam CT) scan to assess available jawbone volume
- Review of diabetes duration: moderately controlled diabetes persisting for more than 10 years may produce complications that diminish tissue health and compromise outcomes
- Vascular complication screening: micro- and macro-vascular complications directly affect healing capacity
- Medication review: certain anti-diabetic medications interact with the healing process and must be factored into the surgical plan
Medications, Antibiotics, and Adjunct Protocols
Clinical evidence supports the use of specific adjunct protocols to improve outcomes in diabetic implant patients:
- Prophylactic antibiotics: dental implants placed in diabetic individuals have proven to be successful when given prophylactic antibiotics, and using 0.12% chlorhexidine increases success even further.
- Bioactive implant surfaces: implant surface features such as bioactive material coatings, greater implant length, and wider diameter have been shown to increase implant success rates in diabetic patients.
- Strict post-surgical monitoring: more frequent follow-up appointments in the first year are standard practice for diabetic patients
- Coordinated care: your implant specialist and endocrinologist or GP should communicate directly to align the surgical timeline with optimal metabolic windows
How to Maximize Your Dental Implant Success- Check List
The steps below are evidence-based and directly actionable. Patients who follow them consistently achieve outcomes that are comparable to non-diabetic individuals.
- ✅ Achieve HbA1c below 8% before surgery — this is the threshold at which implant survival rates align with the general population
- ✅ Treat all periodontal disease first — gum inflammation must be resolved before any implant placement
- ✅ Maintain strict daily oral hygiene — brush twice daily, floss, and use an antiseptic mouthwash
- ✅ Attend all follow-up appointments — early detection of peri-implant mucositis prevents progression to peri-implantitis
- ✅ Avoid smoking — smoking significantly amplifies the already elevated infection and bone loss risks in diabetic patients
- ✅ Follow your diabetes management plan rigorously — stable blood glucose in the weeks surrounding surgery is critical
- ✅ Inform your dental team of all medications — including insulin, metformin, and any supplements
- ✅ Request a multidisciplinary approach — the best outcomes occur when your dental specialist and medical team work in coordination
Frequently Asked Questions (FAQ)
Can I get dental implants if I have Type 2 diabetes?
Yes, in most cases. The overall success rate of dental implants in individuals with Type 2 diabetes is approximately 93.67%, provided glycemic levels are well managed. Your specialist will assess your HbA1c and overall health before recommending treatment.
What HbA1c level is required for dental implants?
Most clinical guidelines recommend an HbA1c below 8% before implant surgery. At this threshold, implant survival rates are comparable to those of non-diabetic patients, ranging from 96.1% to 97.3% at one year.
Does diabetes make dental implants more painful or difficult to heal?
Diabetes can slow wound healing and increase infection risk, but with proper pre- and post-surgical protocols, most patients heal without significant complications. Most implants reach baseline stability within four months, even in moderately uncontrolled diabetic patients, if micro- and macro-vascular complications are absent.
Is Type 1 diabetes a bigger risk than Type 2 for implants?
Yes, according to current data. Implant failures are more likely to occur in Type 1 diabetes patients than in Type 2, with an odds ratio of 4.477 versus 1.777 in comparison to non-diabetic patients. This does not preclude treatment, but it does require a more conservative and closely monitored approach.
How often should diabetic patients have implant check-ups?
More frequently than non-diabetic patients — typically every 3 to 4 months in the first year, then every 6 months thereafter. Regular monitoring allows early detection of peri-implant inflammation, which is far easier to treat in its early stages.
Will my diabetes medications affect the implant procedure?
Some medications may affect healing or interact with anaesthesia. Always provide your dental specialist with a complete list of current medications. In most cases, adjustments are straightforward and do not prevent treatment.