Dental implants have a +97% success rate over 10 years according to decades of peer-reviewed studies – but they are not infallible. Indeed, dental implants can become loose, come off or get infected; which is nothing short of catastrophic considering the investment they represent!
The good news is dental implant failure is easy prevented and, if rapidly detected, is swiftly solved, too. In this article, we take a look at dental implants that failed, learning how to recognize malfunction signs with Dr. Astolfi. Understand what to do if your dental implant fails, and learn about your rights to refunds and full compensation!
How to Know if Something is Wrong with a Dental Implant?
A healthy dental implant should feel like a natural tooth: stable, painless and unremarkable. If it doesn’t, professional check-up is advised as soon as possible.
Your body will usually give you clear signals when an implant is in trouble. Some discomfort in the days after surgery is normal. What is not normal is pain, swelling, or instability that persists.
Early Signs of Implant Failure
If you notice any of the following, contact your dentist without delay:
- Persistent pain or throbbing around the implant site, beyond the first 1–2 weeks post-surgery
- Swollen, red or bleeding gums around the implant
- A loose or wobbly implant — an implant should never move!
- Difficulty chewing
- Bad taste or smell, which may indicate infection
- Visible metal threads
- Swollen lymph nodes in the neck or jaw area
What Do Failed Dental Implants Look Like?
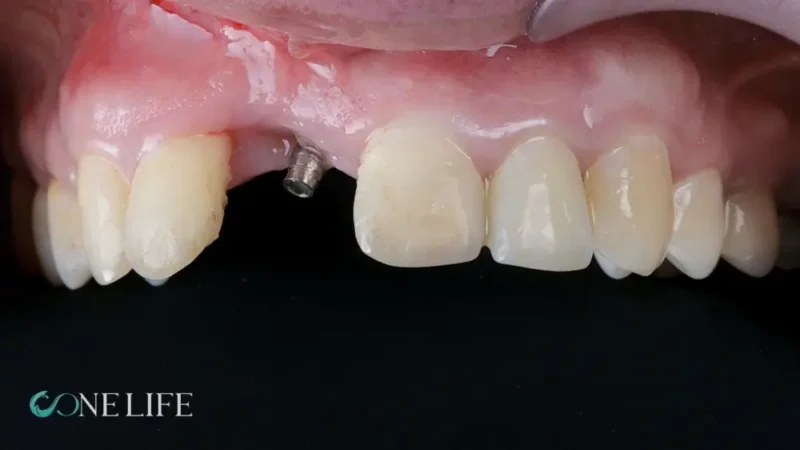
If the gum recedes and you can clearly see the metal threads of the implant, you may be experiencing a failed dental implant due to bone loss. This is one of the most telling visual signs.
Visually, however, a failing implant is not always obvious, especially in its early stages. But there are things you can see:
- Receding gum tissue around the implant, making the metal post partially visible
- Redness and puffiness of the surrounding gum
- Pus or discharge near the implant site
- Visible bone loss on an X-ray, even before symptoms appear
How Common is it for Dental Implants to Fail?
Dental implant failure is rare — but not impossible. Clinical studies consistently show a 97% success rate at 10 years and 75% at 20 years (Jomos), making implants one of the most reliable procedures in modern medicine. A 2024 meta-analysis confirmed that approximately 4 out of 5 implants survive the full 20-year period PubMed(published in Clinical Oral Investigations)
That said, the average failure rate is 3.1% worldwide, rising to approximately 6% in the United States. Impressions Dental These numbers vary depending on the clinic, the patient’s health profile, and the type of implant used.
What is the #1 Risk Factor for Implant Failure?
The single biggest cause of implant failure is infection — specifically peri-implantitis. The good news: peri-implantitis is largely preventable with proper oral hygiene and regular dental check-ups. Early detection is everything.
Main Causes for Dental Implant Failure
Dental implant failure falls into two categories based on when they happen. Early implant failure (happening within the first 3 months post-op), is the most common:
Early Failure | Late Failure | |
Timing | Within the first 3 months | After 3 months or years later |
Main cause | Failed osseointegration (implant doesn’t bond to bone) | Peri-implantitis, mechanical stress, bone loss |
% of all failures | ~83% | ~17% |
Key triggers | Poor bone quality, surgical error, contamination | Poor hygiene, smoking, systemic disease, overloading |
Reversible? | Often yes, with reimplantation | Depends on extent of bone loss |
Patient-Related Risks
Several patient factors significantly raise the likelihood of dental implant failure:
- Smoking: reduces blood flow to the gums
- Uncontrolled diabetes: weakens the immune system and slows osseointegration
- Poor oral hygiene: allows bacteria to accumulate
- Osteoporosis or low bone density: reduces the implant’s structural foundation
- Age over 60: patients in the 60–79 age group have a significantly higher risk of implant failure compared to those under 40 (relative risk: 2.24)
- Certain medications: including bisphosphonates and immunosuppressants
- Heavy alcohol consumption: impairs healing during osseointegration
Clinic-Related Risks
Not all failures are the patient’s fault. Clinical factors matter equally and are often indicative of early implant failure symptoms:
- Incorrect implant sizing or positioning
- Inadequate pre-surgical planning: failing to assess bone volume or density with 3D imaging (CBCT)
- Poor sterilisation protocols: introduces bacteria at the time of placement
- Ill-fitting crowns or prosthetics: creates irritation and inflammation at the implant site
- Insufficient follow-up care: allows early complications to go undetected
*One study found that 83% of failed implants were located in the maxilla, where bone density is typically lower, especially near the sinuses. Bite Club
What Can be Done if a Dental Implant Fails?
If your implant fails, don’t worry: most patients can be successfully retreated. The first step is a clinical assessment including X-rays or a CBCT scan. The cause determines the solution. A failed implant caused by infection requires a different approach than one caused by mechanical overload or poor bone volume.
Implant Replacement Surgery
In most cases, the failed implant is removed, the site is cleaned and allowed to heal, and a new implant is placed — sometimes after bone grafting to rebuild the jaw. Studies show that the 1-year survival rate of reimplanted implants is 89.4%, and when all reimplantation attempts are considered together, the total cumulative survival rate reaches 99.2%. PubMed Central
How Does a Dentist Fix a Failed Implant?
The approach to fixing a failed dental implants depends on the type and extent of failure:
- Early failure with no bone loss→ Remove implant, allow healing (2–3 months), replace
- Peri-implantitis without severe bone loss→ Deep cleaning, antibiotics, possible bone grafting, then re-evaluate
- Significant bone loss→ Bone graft required before any new implant can be placed; timeline extends to 6–12 months
- Mechanical failure (cracked implant, broken abutment)→ Component replacement, sometimes full reimplantation
How Many Times Can a Dental Implant Be Replaced?
There is no limit on the number of times an implant can be treated. Of patients whose second reimplant also failed, a third attempt was made in selected cases, and all of those survived. PubMed Central However, each successive attempt requires careful evaluation of the patient’s bone health, systemic conditions, and the original cause of failure.
Dental Implant Failure After 10 Years
After a decade, the main threats for late implant failure are progressive bone loss, changes in overall health, and mechanical wear. The implant screw itself rarely fails after 10 years — it is usually the surrounding biology (bone and gum tissue). Annual check-ups, including X-rays, are the most effective for catching late-stage problems before they become irreversible.
Who Pays for a Failed Dental Implant?
The responsibility of dental implant failure depends on why it failed and where you had it done. Also: patients have more rights than many realise!
Can I Get a Refund for a Failed Dental Implant?
In many cases, yes — partially or fully. Clinics such as OONE LIFE Dental offer a written guarantee and medical insurance on their implant work, typically covering:
- Free replacement of the implant if it fails
- Free corrective treatment for complications
- Contribution if you are treated elsewhere
Always request a written guarantee before treatment begins. A clinic that is unwilling to put its warranty in writing is a red flag.
Is a Dentist Responsible for a Failed Implant?
If the failure occurs due to poor surgical placement, incorrect implant sizing, or lack of proper sterilisation, the responsibility may fall on the dentist or clinic.
If, however, the failure is linked to patient factors — smoking, poor hygiene, systemic disease — the clinical responsibility is reduced. This is precisely why pre-treatment informed consent forms matter, and why patients should disclose their full medical history before any implant procedure.
In cases of genuine clinical negligence, patients in most countries have the right to pursue a formal complaint or legal claim against the treating dentist or clinic.
Dental Implants in Turkey: Patient Rights, Refunds & Complication Insurance
Turkey is one of the world’s leading destinations for dental implants — offering high-quality care at significantly lower costs. Single dental implants in Turkey typically cost between £300 and £650 ($400 to $800), compared to several thousand in Western countries. But what happens if something goes wrong?
Turkey’s Mandatory Complication Insurance (2026)
Starting from January 2026, all international patients travelling to Turkey for dental treatment are required to obtain complication insurance, under a regulation by the Turkish Ministry of Health.
Hospitals and clinics are responsible for arranging that patients have the required insurance. Notably, a complicationmay occur even when surgery is performed competently — independent of medical error. This means you are protected even when no one is at fault.
What Does Complication Insurance Cover?
The policy covers revision surgery or second operations when a doctor determines is is medically necessary.
Key points to know:
- Coverage period:typically 6 months post-procedure; extended plans may cover up to 12 months
- Where it applies:complications must be treated within Turkey to be eligible for reimbursement
- Who arranges it:the clinic, not the patient
How to Verify a Clinic is Compliant
Before booking, ask the clinic directly:
- Are you registered on theHealthTürkiye platform?
- Do you provide mandatorycomplication insurance for international patients?
- What is your writtenimplant guarantee policy?
- Are you accredited byUSHAŞ (the Turkish Ministry of Health’s health tourism authority)?
A clinic that cannot answer all four questions clearly is not the right choice.
At OoneLife Dental, we are fully compliant with Turkey’s health tourism regulations and provide comprehensive aftercare for every patient.
FAQs
What are signs of dental implant failure?
The most common warning signs are: persistent pain or throbbing beyond the first two weeks after surgery, a loose or wobbly implant, swollen or bleeding gums that don’t settle, bad taste or smell near the implant, visible metal threads due to gum recession, and pus or discharge around the implant site. If you notice any of these, contact your dentist promptly — early intervention dramatically improves outcomes.
Can a dental implant get infected years later?
Yes. Late failures can occur after the implant has been in use for some time, with chronic infections and peri-implantitis among the most common causes.
Can a dentist tell if an implant is failing?
Yes — often before the patient notices any symptoms. A dentist uses dental X-rays or 3D CBCT scans to detect bone loss around the implant, and clinical probing to identify pocket depth and bleeding that indicate peri-implantitis.
What does dental implant failure feel like?
Early failure often presents as persistent, throbbing pain that does not improve after the initial healing phase. Late failure may feel like gradually increasing pressure sensitivity, a subtle looseness when chewing, or recurring soreness around the implant. Some patients describe a dull ache that comes and goes. In cases of infection, there is often a noticeable bad taste or smell.
What is the biggest problem with dental implants?
The most frequent cause of dental implant failure is infection. Peri-implantitis is the single most significant long-term threat to implant survival. The good news is that it is largely preventable with consistent oral hygiene and regular professional maintenance.
How long does it take to know if a dental implant has failed?
Early failure becomes apparent within the first 3 months, when the implant is still integrating with the bone. If the implant is still stable and pain-free after 6 months, the risk of failure drops significantly. That said, late failures can emerge years or even decades after placement.
Can you get another dental implant if one fails?
In most cases, yes. The 1-year survival rate of reimplanted implants is 89.4%, and the overall cumulative survival rate — including second and third attempts — reaches 99.2%.
At what stage do dental implants fail?
Studies show that early failures account for approximately 83% of all implant failures, occurring within the first three months when osseointegration is most vulnerable. Late failures account for the remaining 17%.
Can antibiotics clear up a dental implant infection?
Antibiotics can reduce bacterial load and control the spread of infection, but they cannot reverse bone loss already caused by peri-implantitis. Peri-implantitis is typically treated with a combination of deep cleaning and antimicrobial therapy.
How common are failed dental implants?
The global average failure rate is approximately 3.1%, rising to around 6% in the United States. Rates vary depending on the patient’s health profile, the clinic’s experience, and the quality of aftercare.
What does the 20-year data on dental implant survival show?
The famous 2024 meta-analysis published in Clinical Oral Investigations found that 4 out of 5 implants survive the full 20-year period. PubMed The authors emphasised that long-term follow-up care is essential and should not end after 10 years.
How do they remove a failed dental implant?
Removal is a minor surgical procedure performed under local anaesthetic. The dentist or oral surgeon uses a specialised instrument — typically a reverse-torque device or piezosurgery tool — to unscrew or carefully loosen the implant from the surrounding bone. In cases where the implant is not integrated (early failure), removal is straightforward. Where osseointegration has partially occurred, the process requires more care to preserve the surrounding bone for future reimplantation.

