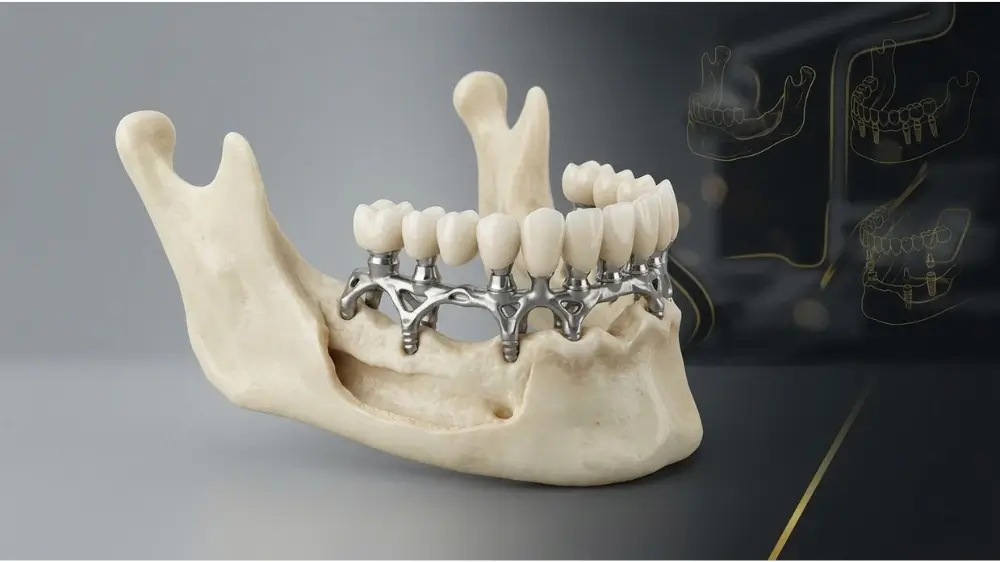
A subperiosteal implant sits directly on top of the jawbone but underneath the gum tissue, providing a stable foundation for patients with severe bone loss. Modern designs have evolved from the 1940s; today, they are engineered using high-precision digital workflows to ensure a microscopic fit that promotes healthy tissue and long-term prosthetic support.
What are Subperiosteal Implants?
A subperiosteal implant is the primary alternative for treating atrophic maxillae and mandibles where the bone has resorbed significantly due to long-term tooth loss, trauma, or disease. By using 3D imaging and biocompatible materials like medical-grade titanium, laboratories create a personalized fit that distributes occlusal forces across the jaw.
- Unilateral Subperiosteal: Designed to replace teeth in a specific quadrant of the mouth where bone loss is localized.
- Circumferential (Full Arch): A complete framework that spans the entire upper or lower jaw to support a full bridge or overdenture.
- Tripodal Design: Engineered to distribute pressure across three strategic points of the jaw to maximize stability and minimize stress on thinner bone sections.
Main Advantages
Subperiosteal dental implants provide a fixed dental solution for patients with extreme bone atrophy without the need for bone grafting.
- Reduced Treatment Time: Unlike traditional implants combined with bone grafts—which can take 6 to 12 months to heal—subperiosteal implants often support a prosthesis much sooner.
- Minimal Surgical Invasiveness: Because there is no need to harvest bone from the hip or chin, or to perform complex sinus lifts.
- Custom Digital Precision: Each framework is 3D-engineered to fit the exact topography of your jaw, ensuring a predictable fit that implants cannot match.
- Broad Load Distribution: The framework distributes the pressure of chewing across a larger surface area, preventing localized stress on fragile bone structures.
Who is it Recommended for?
A subperiosteal implant is recommended when a patient has suffered significant alveolar bone resorption and is unwilling or medically unable to undergo extensive bone augmentation. This typically occurs in patients who have been edentulous (toothless) for many years or those who have experienced trauma or severe periodontal disease.
Clinical indications for a subperiosteal recommendation include:
- Severe Maxillary or Mandibular Atrophy: When the vertical height or horizontal width of the bone is insufficient to house even “short” or “narrow” traditional implants.
- Bone Graft Failure: Patients who have previously attempted bone grafts or sinus lifts that did not successfully integrate.
- Medical Contraindications for Grafting: Situations where a patient’s systemic health makes long healing periods or multiple surgeries for grafting less ideal.
- Desire for Faster Results: Patients looking for a functional, fixed bridge without the year-long wait associated with reconstructive bone surgery.
The 5-Step Procedure
The surgical placement of a subperiosteal implant is a specialized procedure that typically involves a single stage, thanks to modern CAD/CAM digital planning. At our clinics, we ensure the process is as streamlined and comfortable as possible for the patient.
- Digital Diagnostics: We begin with a high-resolution CBCT scan. This allows us to map the bone density and the path of the inferior alveolar nerve or the position of the maxillary sinuses.
- Surgical Access: Under local anesthesia or IV sedation, a precise incision is made in the gingival tissue to expose the underlying bone ridge.
- Framework Placement: The custom-made titanium subperiosteal framework is placed directly onto the bone. Because it was designed from the patient’s 3D data, it “snaps” into place with high passive fit.
- Fixation: Small prosthetic screws may be used to provide initial stability while the soft tissues heal over the framework.
- Suturing: The gums are closed around the protruding “posts” or abutments, which will eventually hold the dental bridge.
Recovery After Subperiosteal Implants
Recovery after subperiosteal implants typically takes between 7 to 14 days for initial soft tissue healing, though complete integration can take several months.
- First 48 Hours: Expect mild swelling and bruising. Cold compresses and prescribed anti-inflammatories are usually sufficient to manage discomfort.
- Dietary Restrictions: A soft-food diet is mandatory for the first 4 to 6 weeks to avoid putting excessive “masticatory load” on the framework while the gums heal.
- Oral Hygiene: Patients must use specialized antimicrobial rinses. Brushing the surgical site is avoided for the first few days to prevent trauma to the sutures.
- Prosthetic Loading: In many cases, a temporary bridge can be fitted shortly after surgery, but the final, permanent prosthesis is typically placed once the soft tissues are fully matured.
What Are the Complications of Subperiosteal Implants?
Subperiosteal implants carry specific clinical risks that must be managed by an experienced oral and maxillofacial surgeon. Potential risks include:
- Gingival Dehiscence: This occurs when the gum tissue over the framework opens, exposing the metal. This is the most frequent complication in highly atrophic jaws.
- Infection (Peri-implantitis): Because the framework covers a large surface area, an infection can spread along the metal-bone interface if strict hygiene is not maintained.
- Framework Instability: If the 3D design was not perfectly adapted to the bone topography, the implant may shift, leading to discomfort or prosthetic failure.
- Nerve Paresthesia: Although rare with 3D CAD/CAM planning, the proximity to the mental nerve in the mandible requires extreme surgical precision.
How Much Does a Subperiosteal Implant Cost?
In the United States, a subperiosteal dental implant typically costs between $4,000 and $6,000 per unit for localized rehabilitation, while a full-arch subperiosteal restoration ranges from $25,000 to $50,000. This price is all-inclusive of the custom CAD/CAM 3D-milled titanium framework, the specialized surgical placement, and the high-end prosthetic teeth.
Cost Breakdown:
- Custom Engineering & 3D Fabrication: Approximately $1,500 – $2,500. This covers the high-resolution CBCT analysis and the manufacturing of the biocompatible titanium frame tailored to your bone topography.
- Surgical Placement & Clinical Fees: Approximately $2,000 – $3,500. This includes the specialized surgeon’s time, sterile environment, and local or IV sedation.
- Final Prosthetic Restoration: Approximately $1,500 – $3,000 per quadrant. This is the visible part of your smile—the high-durability teeth that attach to the framework.
Treatment Scope | Estimated US Cost (2026) | Included Services |
Localized (1-3 Teeth) | $4,500 – $7,500 | Framework + Custom Crowns |
Single Arch (Upper or Lower) | $25,000 – $45,000 | Full 3D Framework + Fixed Bridge |
Full Mouth (Both Arches) | $45,000 – $85,000 | Dual Frameworks + Full Rehabilitation |
Success Rates and Durability
The clinical success rate for modern 3D-designed subperiosteal implants is approximately 93% to 98% over a 5-to-10-year period. While early versions from the 1960s had mixed results due to manual fitting, today’s CAD/CAM technology ensures a microscopic fit.
Long-term durability depends heavily on three factors:
- Bone Health: Although used in “atrophic” (thin) bone, the remaining bone must be stable and free of active disease.
- Soft Tissue Management: The health of the gums over the metal framework is the most critical factor for longevity.
- Patient Maintenance: Regular professional cleanings are non-negotiable, as plaque can still accumulate around the metal “posts” that emerge from the gums.
What is the Alternative? Subperiosteal Implants vs. Bone Grafting
Choosing between a subperiosteal implant and a traditional implant with bone grafting depends on the patient’s anatomy, health history, and timeline. The following table highlights the key differences:
Feature | Subperiosteal Implant | Bone Grafting + Endosteal Implant |
Total Treatment Time | 2–4 months | 9–15 months |
Number of Surgeries | Usually 1 | 2 to 4 |
Surgical Invasiveness | Moderate (Surface of bone) | High (Bone harvesting/augmentation) |
Success in Severe Atrophy | High | Variable (Graft resorption risks) |
Healing Complexity | Lower systemic demand | High (Requires active bone growth) |
Customization | 100% Patient-Specific (3D) | Standard sizes |
FAQs
Are subperiosteal implants still used today?
Yes, subperiosteal implants have seen a significant clinical revival in 2025 and 2026 due to 3D printing technology.While they fell out of favor in the 1990s, the ability to custom-mill titanium from a CBCT scan has solved the fitting issues of the past. They are now considered a premier “salvage” option for severe atrophy.
How long do subperiosteal implants last?
With proper maintenance, modern subperiosteal implants are designed to last 15 to 25 years. Data from 2026 show that while the titanium frame itself is nearly indestructible, the longevity of the restoration depends on the health of the overlying gums and the patient’s systemic health.
What is the success rate of subperiosteal implants?
The current success rate for CAD/CAM-designed subperiosteal implants is approximately 98% for the first three years. This high predictability is attributed to Selective Laser Melting technology, which allows for a porous surface on the titanium that promotes better “soft-tissue anchoring.”
What are subperiosteal implants made of?
Subperiosteal implants are primarily made of medical-grade Titanium (Grade 5) or Cobalt-Chrome alloys.Titanium is the gold standard in 2026 because it is biocompatible, lightweight, and allows for the 3D additive manufacturing required to match your jaw’s unique topography.
Are subperiosteal implants worth it?
Subperiosteal implants are worth it for patients who want to avoid the 12-month wait and high cost of multiple bone grafts. They provide a fixed, non-removable bridge in cases where traditional implants would simply fail due to lack of bone.
Are subperiosteal implants painful?
The procedure is performed under local anesthesia or IV sedation, meaning you will feel no pain during the surgery. Post-operative discomfort is typically managed with standard anti-inflammatories and is often described as less painful than a sinus lift or a hip-bone harvest.
What are the disadvantages of Subperiosteal implants?
The primary disadvantage is the risk of “dehiscence,” where the metal framework may become exposed if the gum tissue is too thin. Additionally, they require a highly specialized surgeon and a higher upfront cost for the custom 3D design compared to standard off-the-shelf screws.