The osseointegration of a dental implant is the fusing of jawbone and an implant. Without this, an implant would be a foreign object that the body would eventually reject. Dentistry relies on this integration to ensure long-term implant success rates. When successful, the bond is so strong that the implant can withstand the mechanical forces of chewing and biting, often outlasting natural teeth if maintained correctly.
How does osseointegration work?
Through the direct attachment of bone-forming cells to the implant surface, osseointegration creates a stable biological union without any intermediate connective tissue. This interface provides the foundation to support dental implants.
How long does the osseointegration of dental implants take?
Typically, the osseointegration timeline takes 3 to 6 months. Factors such as bone density, implant material and implant location—upper or lower jaw— impact healing duration. Below, we go through each in detail.
Lower vs Upper Jaw Osseointegration Time
The mandible (lower jaw) usually integrates faster, often around 3 months, compared to the maxilla (upper jaw). The maxilla may require up to 6 months due to its softer and more porous bone structure.
Osseointegration Time based on the Implant Material
For patients with osteoporosis, bone remodeling is slower. The material and surface treatment of the implant are critical in determining how long this process takes:
- Standard Titanium Implants: In a patient with osteoporosis, standard titanium may require a healing window of 6–9 months. Because the bone is softer, it needs extra time to switch from being held by a screw to being held by a bone.
- Hydrophilic (Active) Titanium Surfaces: These implants “attract” bone cells to speed up healing. For patients with lower bone density, this can fast-track the process to 3–4 months.
- Zirconia (Ceramic) Implants: Zirconia is a body-friendly material (often used when the patient is unable to have titanium implants due to metal allergies etc. ), however it takes 6+ months to fully heal.
Bone Density Classifications and Healing Timelines
D1 Bone: High Density (Mainly Cortical)
- Location: Usually found in the front of the lower jaw (anterior mandible).
- Osseointegration Time: 3–4 Months.
- The Dynamics: D1 bone provides incredible primary stability (it holds the screw very tightly). However, because it is so dense, it has a lower blood supply than softer bone. This means you must be careful not to overheat the bone during surgery, as “burned” bone won’t integrate.
D2 & D3 Bone: Balanced Density (Porous Cortical/Dense Trabecular)
- Location: Common in the posterior lower jaw and anterior upper jaw.
- Osseointegration Time: 4 Months.
- The Dynamics: This is often considered the “Goldilocks” zone for dental implants. It offers enough density for a secure fit but has enough blood vessels to speed up the proliferative phase of bone healing.
D4 Bone: Low Density (Soft/Spongy)
- Location: Typically found in the posterior upper jaw (near the sinuses).
- Osseointegration Time: 6+ Months.
- The Dynamics: D4 bone is like “Styrofoam.” It provides very little initial mechanical grip. Surgeons use tapered implants to “squeeze” and firm up soft bone. As the bone is less solid, the body needs extra time to build a strong network to handle the pressure of biting.
Three Critical Stages of Bone Healing
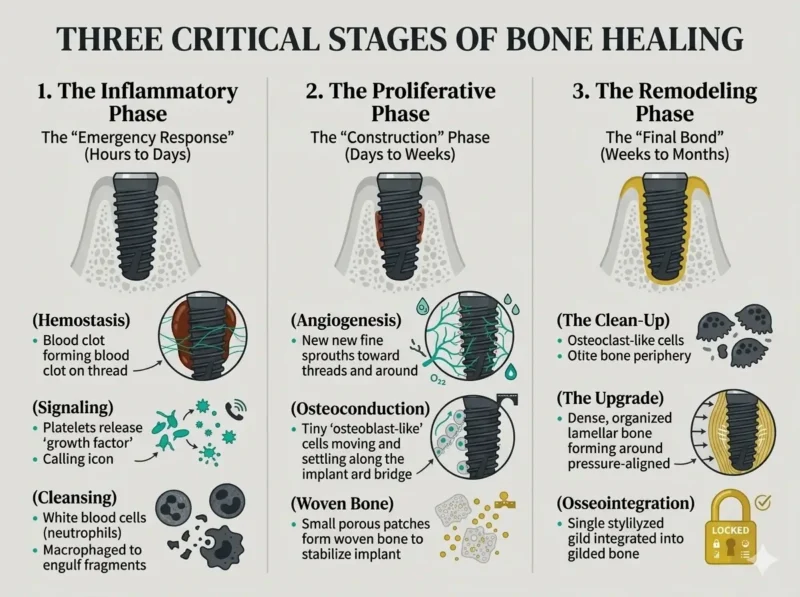
1. The Inflammatory Phase (Hours to Days)
This stage begins when the implant is placed. It is the body’s “emergency response” to surgery.
- Hemostasis: Within seconds, a blood clot forms around the implant. It’s a biological scaffold rich in fibrin that acts as a highway for future cells.
- Signaling: Platelets in the clot release “growth factors” (like PDGF and TGF-beta). These act as chemical beacons, calling out to the immune system and bone-building cells to start the repair work.
- Cleansing: White blood cells (neutrophils and macrophages) arrive to clear out the bacterias or tiny bone fragments created during the drilling process.
2. The Proliferative Phase (Days to Weeks)
This is the “construction” phase, temporary blood cloth replaces with actual tissue.
- Angiogenesis: New blood vessels begin to sprout (neovascularization). This is vital because bone cannot grow without a constant supply of oxygen and nutrients.
- Osteoconduction: The cells use the implant as a bridge to get into position, then they make a foundation that will harden into bone.
- Woven Bone Formation: The body builds a bone to grab onto the implant. It’s not strong yet, but it acts like the initial glue that keeps the implant from moving.
3. The Remodeling Phase (Weeks to Months)
This is when your bone finishes its “renovation” to become rock-solid.
- The Clean-Up: Your body’s “demolition crew” (osteoclasts) dissolves the weak and temporary bone.
- The Upgrade: The “builders” (osteoblasts) lay down lamellar bone. This bone is organized, dense, and built to handle the pressure of chewing.
- The Final Bond: The implant is now “locked” into the jaw. Your body treats it as part of itself, completing the permanent bond.
Factors of Osseointegration Influencing Dental Implant Success Rates
Dental implants boast a global success rate of 95% to 98%. However, the quality of osseointegration—and thus the success of the implant—is influenced by several key data-driven factors:
- Surface Roughness (Micromorphology): Research shows that implants with “sandblasted and acid-etched” surfaces (SLA) increase the bone-to-implant contact (BIC) by up to 60–80% compared to smooth surfaces.
- Surgical Heat Control: Bone cells (osteocytes) begin to die if the temperature during drilling exceeds 47°C (117°F). Precision cooling and low-speed drilling are vital.
- Micromovement Threshold: For successful osseointegration, the implant must not move more than 50–150 microns during the healing phase. Movements larger than this cause the body to form soft scar tissue instead of bone, leading to implant failure.
- Loading Protocols: While “teeth in a day’’ is popular, studies show that ” waiting 3–6 months provides a slightly higher success rate in patients with compromised bone density.
Risk Factors That Can Compromise Integration
- Smoking 🚭: Reduces blood flow and oxygen to the bone, significantly increasing failure rates.
- Diabetes 🩸: Uncontrolled blood sugar can slow the body’s inflammatory response.
- Medications 💊: Certain osteoporosis treatments (like bisphosphonates) must be discussed with your surgeon as they affect bone turnover.
- Gum Disease (Periodontitis) 🦷: Just like a house needs healthy soil, an implant needs healthy gums. Uncontrolled bacteria in the mouth can attack the bone around the implant before it even has a chance to settle, leading to early failure
FAQs
How do I know if my implant is osseointegrated?
You usually can’t tell just by looking, but your dentist will check for stability. If the implant doesn’t move at all and there is no pain when they tap it, it has successfully “bonded” to your bone.
How can I speed up osseointegration?
The best way is to give your “builder cells” the right environment. This means not smoking, managing your blood sugar if you have diabetes, and potentially using “high-tech” titanium implants that act like a magnet for bone cells.
What are the downsides of osseointegration?
The main “downside” is patience. You can’t rush biology. If you put too much pressure on the implant before the “wet cement” (osteoid) turns into “hard bone,” the bond can fail.
How do you eat during osseointegration?
Think “Soft Food Only” for the first few weeks. Stick to things like smoothies, yogurt, eggs, or pasta. You want to avoid any “rattling” or heavy biting that could disturb the builder cells while they are laying the foundation.
What vitamins help osseointegration?
Vitamin D and Calcium are the MVPs. Vitamin D helps your body actually absorb the calcium needed to turn that soft “woven bone” into the rock-hard “lamellar bone” required for chewing.
Does osteoporosis mean I can't get an implant?
Not at all! It just means your healing “window” might be longer—typically 6–9 months instead of 3. Your surgeon might also use a “tapered” implant to get a better grip on the softer bone.
Why is smoking so bad for the bond?
Smoking shrinks your blood vessels, cutting off the “supply line” of oxygen and nutrients. Without these supplies, your “builder cells” can’t survive or work fast enough to lock the implant in place.
What is the "Clean-Up Crew" (Osteoclasts)?
Before your body builds the final, strong bone, it sends in a demolition team to dissolve the weak, messy “quick-dry” bone. This makes room for the high-quality bone that can handle the pressure of an apple or a steak.
What is the difference between Titanium and Zirconia?
Titanium is like a “smart metal” that can be coated to attract cells faster. Zirconia is a beautiful, metal-free ceramic that is super safe but usually follows a slower, traditional healing path of 6+ months.
Can the bond fail later on?
Yes, but it’s usually due to gum disease. Just like a real tooth, if bacteria get under the gums and eat away at the bone, the implant will lose its “grip.” Good brushing and flossing are still essential!

